Systematic review of mental health problems and migration stressors among Kurdish migrants in western host countrie
Published in Behavioural Sciences & Psychology

Why we wrote this
Kurds are one of the world’s largest stateless peoples. Many have faced war, persecution, and repeated displacement. Yet their mental-health needs in Western host countries are rarely synthesized in one place. Our goal was simple: bring together what the research shows so services and policymakers can respond better.
What the research says in plain language
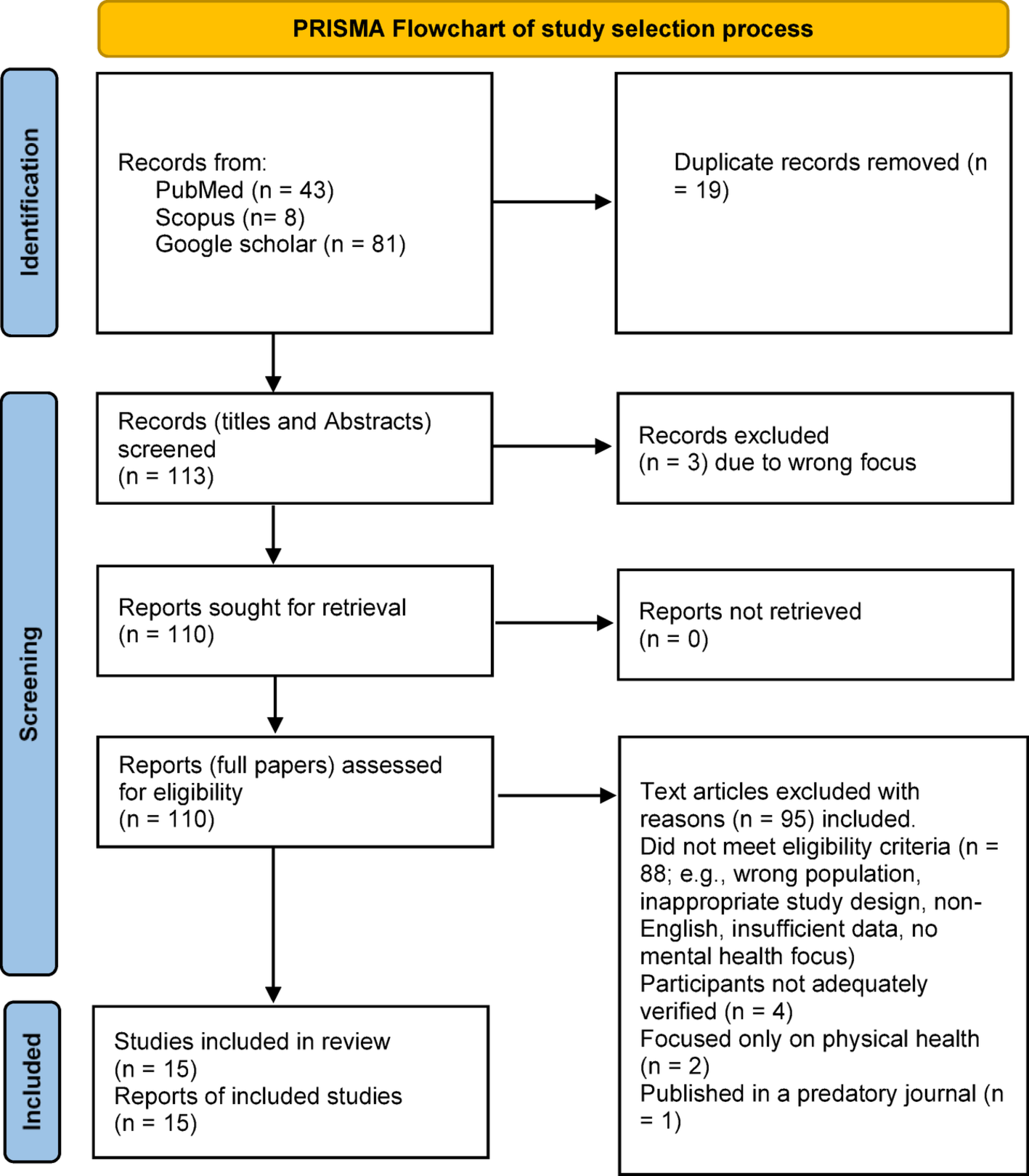
Across the studies we reviewed, totaling 5,319 participants, Kurdish migrants commonly experience substantial psychological distress after resettlement. Reported rates were about 37% for PTSD, 36% for depression, and 28% for anxiety alongside insomnia, fatigue, and, in some cases, suicidal thoughts. These levels reflect both past trauma and new stressors after arrival.
Before migration
Most people left because of war and political oppression, violence and persecution, and economic hardship. These are not abstract labels; they translate into lived experiences of fear, loss, and disruption that shape mental health for years.
After migration
Trauma doesn’t end at the border. Many face discrimination, isolation and loneliness, family separation, economic difficulties, and fear of deportation. These chronic stressors can sustain or worsen mental-health problems if left unaddressed.
What needs to change
-
Care that fits culture and context. Kurdish-language support, trusted community spaces, and services co-designed with Kurdish organizations can reduce stigma and improve engagement.
-
Legal and social help alongside clinical care. Link mental-health services with legal aid, housing, employment, and family-reunification pathways; these determinants strongly influence recovery.
-
Continuity when status is uncertain. For those facing return, plans for continuity of care and cross-border referrals are essential.
What surprised us
Despite different host-country policies, high distress appeared consistently. Legal uncertainty especially fear of deportation was a recurring theme linked to anxiety and sleep problems.
Where we go from here
We need longitudinal studies, better measurement of post-migration stressors, and interventions that integrate mental-health care with settlement services. Most importantly, Kurdish communities should be partners not just participants in designing solutions.
Follow the Topic
-
Discover Mental Health
This is an international, open access journal that publishes research across the transdisciplinary field of mental health research.
Your space to connect: The Psychedelics Hub
A new Communities’ space to connect, collaborate, and explore research on Psychotherapy, Clinical Psychology, and Neuroscience!
Continue reading announcementRelated Collections
With Collections, you can get published faster and increase your visibility.
Neurocognitive Disorders Beyond Cognition: Behavioral, Psychological, and Social Dimensions
Neurocognitive disorders, including mild cognitive impairment (MCI) and dementia, are defined by cognitive decline. However, their clinical reality extends far beyond cognitive symptoms. Behavioral and psychological manifestations are highly prevalent, and often more distressing for patients and caregivers than cognitive decline itself. These symptoms accelerate functional deterioration, increase caregiver burden, and contribute to poor quality of life and higher healthcare costs.
This Special Collection seeks to highlight the behavioral, psychological, and social dimensions of neurocognitive disorders, bridging biological mechanisms, clinical management, psychosocial outcomes, and health policy. In particular, it aims to explore how the digital health and policy innovations can make a meaningful impact.
We invite research that explores how digital health, AI, and telemedicine can advance assessment, intervention, and care models, as well as studies that inform policy and service delivery. Submissions may include original research, systematic reviews, methodological papers, and policy analyses from psychiatry, neurology, psychology, geriatrics, and related fields.
Scope
1. Behavioral and Psychological Symptoms – Neuropsychiatric manifestations (e.g., depression, apathy, agitation, aggression, delusions, hallucinations) in dementia and MCI, their mechanisms, clinical correlates, and psychosocial Impact (e.g., on quality of life, caregiver burden, stigma, social participation).
2. Interventions – Pharmacological, psychosocial, lifestyle-based, and digital interventions (e.g., app-based therapies, AI-assisted care) targeting behavioral, psychological, and social needs.
3. Policy and Care Models – Service innovations and policy frameworks, including the integration of digital platforms, AI-supported systems, and telemedicine in dementia and MCI care.
Keywords: dementia, major neurocognitive disorder, mild neurocognitive disorder, mild cognitive impairment, behavioral and psychological symptoms of dementia, Neuropsychiatric manifestations
Publishing Model: Open Access
Deadline: Jun 15, 2026
Mental Health across the Lifespan: From Childhood to Late Adulthood
Mental health is a universal concern impacting individuals at every stage of life, influenced by a complex mix of biological, psychological, and social elements that shift as people age. Each phase from early childhood and adolescence through adulthood to older age presents unique mental health challenges, protective factors, and opportunities for early intervention. Early childhood and adolescence are crucial periods for identifying mental health issues as they emerge and for implementing preventive strategies that can shape outcomes well into later life. During adulthood, individuals commonly encounter stressors related to work, relationships, parenting, and identity development, which can trigger or exacerbate conditions such as anxiety, depression, substance use disorders etc. In later life, older adults face additional challenges like cognitive decline, social isolation, grief, chronic health problems, and loss of independence, all of which can profoundly impact mental wellbeing. Although awareness of the importance of a lifespan perspective in mental health is increasing, much research remains fragmented and focused on specific age groups. This segmentation limits comprehensive understanding of mental health across the entire life course. To bridge this gap, there is a critical need for integrated, longitudinal, and comparative research that tracks mental health trajectories, identifies risk and protective factors, evaluates access to care, and assesses age appropriate interventions. This special issue aims to consolidate interdisciplinary and international insights on mental health through a lifespan lens. It welcomes original research, systematic reviews, theoretical models, and case studies that explore mental health progression, age specific challenges, and intergenerational influences on psychological wellbeing.
Sub themes:
• Mental health issues in childhood and adolescence
• Early life and the role of the social environment
• Adverse childhood experiences and mental health
• Prevention and early intervention in youth mental health
• Mental health challenges in early adulthood
• Psychological wellbeing at the workplace
• Mental health in midlife
• Emotional adjustment during midlife transitions
• Mental and cognitive wellbeing in older adulthood
• Grief, loneliness, and social isolation in later life
• Ageism, stigma, and their impact on mental health
• Psychological support and emotional care at end of life
• Generational differences and its influence on mental health
Keywords: Mental health, lifespan perspective, age specific challenges, preventive strategies, protective factors, early intervention
Publishing Model: Open Access
Deadline: Jun 09, 2026



Please sign in or register for FREE
If you are a registered user on Research Communities by Springer Nature, please sign in