The future of noninvasive glucose monitoring is in your smartwatch
Published in Healthcare & Nursing

By Brinnae Bent, PhD and Jessilyn Dunn, PhD
BIG IDEAs Lab, Duke University Departments of Biomedical Engineering and Biostatistics & Bioinformatics
Glycemic health is at an all-time low: in the U.S., one in ten people have diabetes and one in three people have prediabetes. Prediabetes is often poorly managed, which leads to 70% of individuals with prediabetes eventually developing type 2 diabetes (T2D). However, it’s not all bad news; Promisingly, prediabetes is reversible with lifestyle modifications: the Diabetes Prevention Program reduced diabetes incidence by 58% through interventions aimed at weight loss, dietary change, and physical activity in patients with prediabetes. In order to manage glucose fluctuations, it is important for people to understand how their behaviors influence their blood glucose levels. There is a critical need for innovative, practical strategies to improve monitoring and management of glycemic health.
This critical need for accessible strategies to monitor glycemic health motivated our recent study, where we developed a proof of concept for developing digital biomarkers of glycemic health from noninvasive, wrist-worn wearables and food logs.
Using a dataset of 25,000 simultaneous interstitial glucose and noninvasive wearable smartwatch measurements, we demonstrated the feasibility of using noninvasive and widely accessible methods, including smartwatches and food logs recorded over 10 days, to continuously detect personalized glucose deviations and to predict the exact interstitial glucose value in real time with up to 84% and 87% accuracy, respectively (Figure 1).

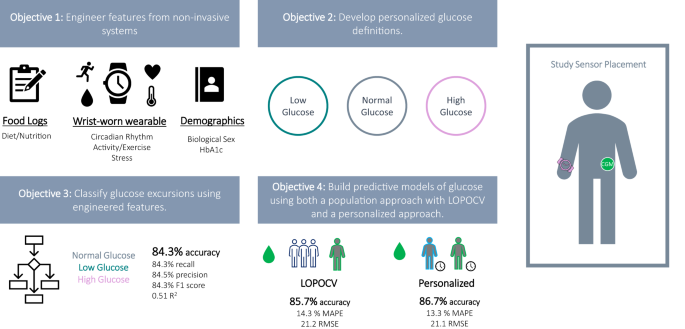
Figure 1.This study has four objectives: 1) Engineer features from non-invasive systems using a combined data-driven and domain-driven feature engineering approach. 2) Develop personalized glucose excursion definitions. 3) Classify glucose excursions using engineered features. 4) Build predictive models of glucose using both a population approach with leave-one-person-out cross validation and a personalized approach.
In this study, we contributed three primary findings to propel the field of noninvasive glucose monitoring forward:
- Developed a method for classifying intra-individual glucose excursions. In layman’s terms, this means that we are detecting when a person’s glucose level is abnormal as compared to their own usual glucose levels. Previous definitions of glucose excursions were developed for diabetes management and may not be adequate to explain glucose deviations in individuals with prediabetes and normal HbA1c because of lower fasting glucose levels and lower glucose variability than in those with diabetes. Personalization of glycemic health has also previously been shown to be very important when describing intra-individual differences in glycemic response, likely because physiological response to diet, exercise, stress, and other lifestyle factors vary widely among individuals.
- Built a proof-of-concept method for completely noninvasive glucose prediction using a smartwatch and food logs, demonstrating robust classification of personalized interstitial glucose excursions from non-invasive wearables and food logs (Figure 2)and creating a noninvasive continuous glucose monitor “proxy” with high accuracy.
- Implemented novel feature engineering methods that achieve high accuracy in interstitial glucose classification and regression models. These features highlight the existence of important relationships between physiologic measurements from non-invasive wearables and interstitial glucose fluctuations, which serves as a basis for future experimental studies (figure 2).
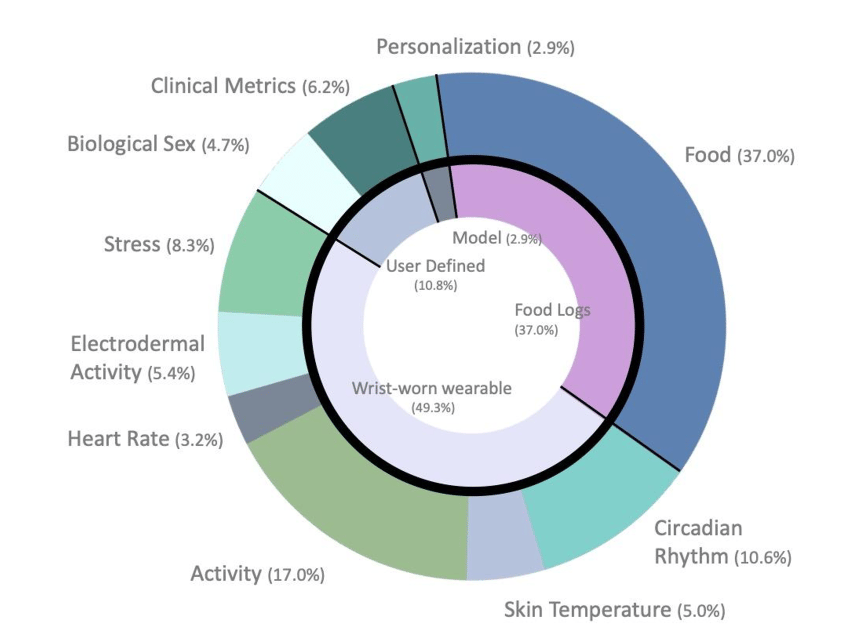
Figure 2. Importance of 69 domain-driven and data-driven features in glucose predictions. Importance was determined from a random forest feature selection model using impurity-based feature selection. The outer circle shows the relative contribution of food, circadian rhythm, activity, stress, gender, clinical metrics, personalization, electrodermal activity, heart rate, and skin temperature to the accuracy of the models. The inner circle shows the relative importance by source of features, including food logs, the wrist-worn wearable, user-defined features, and features defined for/by the model.
In this study, we determined that it is possible to build models from noninvasive wearables data combined with food logs to classify interstitial glucose levels and to predict interstitial glucose. This novel, noninvasive method to monitor interstitial glucose in real time may provide a powerful and frictionless option for people to engage with their glycemic health and actively monitor the effects of behavioral change. Read more: https://www.nature.com/articles/s41746-021-00465-w
Follow the Topic
-
npj Digital Medicine
An online open-access journal dedicated to publishing research in all aspects of digital medicine, including the clinical application and implementation of digital and mobile technologies, virtual healthcare, and novel applications of artificial intelligence and informatics.
Related Collections
With Collections, you can get published faster and increase your visibility.
Evaluating the Real-World Clinical Performance of AI
Publishing Model: Open Access
Deadline: Jun 03, 2026
Impact of Agentic AI on Care Delivery
Publishing Model: Open Access
Deadline: Jul 12, 2026

Please sign in or register for FREE
If you are a registered user on Research Communities by Springer Nature, please sign in