The genetic contribution of genetics to food addiction
Published in Chemistry, Genetics & Genomics, and General & Internal Medicine
This study emerged from a fundamental puzzle in eating-behaviour research: why do some individuals with obesity exhibit patterns of compulsive food consumption and psychological symptoms that resemble addiction, while others with similar body mass index (BMI) do not? Although the concept of food addiction has gained interest in recent decades, it remains controversial and poorly understood, especially at a biological level. Traditional explanations often focus on calorie balance, environmental exposure to processed foods, or psychosocial stressors alone. With this study we wanted to integrate genetic mechanisms into this broader picture to see whether variation in genes known to regulate appetite and reward might help explain individual differences in addictive-like eating behaviour.
The investigation focuses on the melanocortin-4 receptor (MC4R) gene, which plays a key role in the brain’s regulation of satiety, reward, and energy balance. Prior studies have linked MC4R variants to obesity and eating behaviours, but direct genetic associations with clinically defined food addiction had not yet been rigorously tested among people with obesity. By genotyping multiple MC4R polymorphisms (including rs17782313) in a clinical sample of people seeking weight-loss treatment and comparing those with versus without food addiction based on validated diagnostic scales, our group aimed to bridge molecular variation with behavioural phenotype.
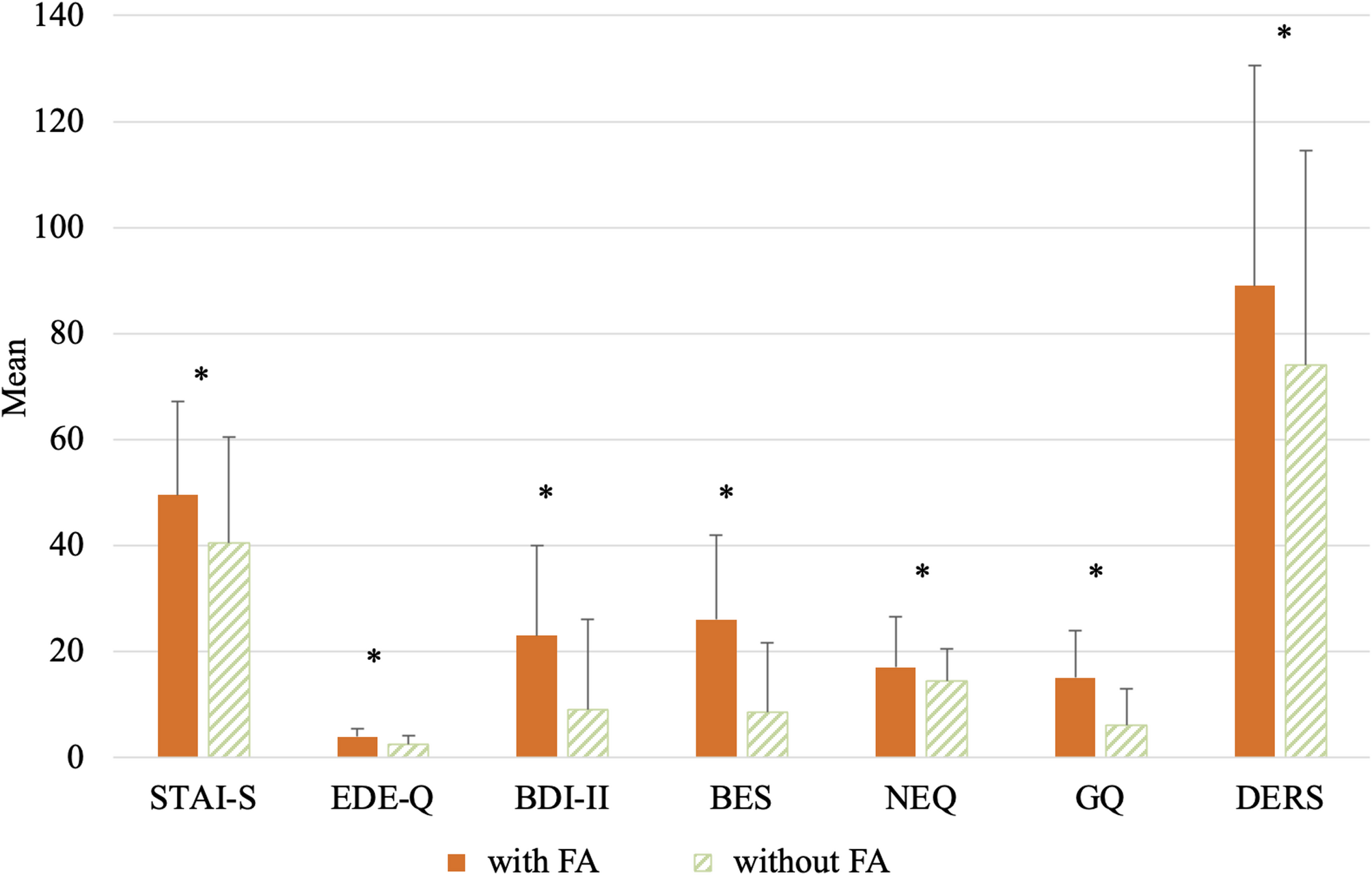
The main finding was relevant: one MC4R variant (rs17782313) showed a robust association with food addiction. Specifically, carriers of the C allele were not only more likely than non-carriers to meet criteria for food addiction, and, noteworthy, they also had higher levels of anxiety and depressive symptoms, dimensions that are often intertwined with compulsive eating.This finding suggests that genetic variation in a key appetite regulation pathway contributes not only to patterns of loss of control over eating but also to associated affective symptoms.
Scientifically, these results underscore that eating behaviours and obesity are not reducible to simple external factors or conscious decision making alone. Instead, individual biological predispositions interact with psychological and environmental influences to shape how people respond to food rewards and regulate intake. The results encourage moving beyond a purely behavioural or environmental framing of obesity, positioning genetic insights as a tool for more nuanced risk stratification and potentially tailored interventions.
From a clinical point of view, the study stresses the importance of recognizing heterogeneity within obesity as some patients may struggle with patterns resembling addiction because of inherent differences in reward-related circuitry, not just lifestyle or willpower. Understanding these peculiarities can help refine assessment, reduce stigma, and design supportive interventions that account for underlying biological vulnerabilities.
In essence, the paper invites the clinicians and researchers to rethink food addiction from a metaphor derived from substance use to a genetic-informed behavioural phenotype that, if validated in future studies, could link molecular neuroscience with real-world therapeutic strategies.
Follow the Topic
-
Journal of Eating Disorders
This is the first Gold open access, peer-reviewed journal publishing leading research in the science and clinical practice of eating disorders.
Related Collections
With Collections, you can get published faster and increase your visibility.
Not a Monolith: Identifying Meaningful Heterogeneity in Eating Disorder Symptoms Among LGBTQ+ Populations
Eating disorders within LGBTQ+ populations do not follow a singular pattern; instead, they reflect a rich and complex interplay of identities, lived experiences, and social contexts that demand nuanced, intersectional inquiry. This Collection seeks to identify meaningful heterogeneity in eating disorder symptoms by examining diverse identities, lived experiences, social group memberships (e.g., clan membership, subcultural appearance identifications, sexual self-labelling), and the role of various social contexts that LGBTQ+ populations occupy to better capture variations in eating disorder symptoms within this community.
Building on this foundation, this Collection investigates unique risk factors, including, but not limited to, sexual and gender minority stress, intraminority stress, and structural stigma, which may contribute to the development or exacerbation of eating disorder symptoms in LGBTQ+ populations. Equally important is the exploration of protective factors—such as community connectedness and pride in identity—that may buffer against these risks and promote interpersonal and psychological strengths.
Finally, this Collection emphasizes the need for prevention and treatment strategies that are culturally competent, inclusive, and responsive to the specific needs of LGBTQ+ populations. By advancing research in these areas, we aim to improve health outcomes and reduce health disparities in eating disorders among the LGBTQ+ community.
We invite researchers to contribute to this special Collection. Topics of interest within LGBTQ+ populations include, but are not limited to:
-Intersectionality and eating disorders
-Identity-based heterogeneity in symptom presentation
-Sexual and gender minority stress
-Intraminority stress
-Structural stigma and its impact on eating disorder risk
-Protective factors such as community connectedness and identity pride
-Prevention strategies tailored for LGBTQ+ individuals
-Inclusive and culturally responsive treatment approaches
-Case studies on diverse experiences in care and recovery
This Collection supports and amplifies research related to SDG 3, Good Health and Well-Being.
All submissions in this collection undergo the journal’s standard peer review process. Similarly, all manuscripts authored by a Guest Editor(s) will be handled by the Editor-in-Chief. As an open access publication, this journal levies an article processing fee (details here). We recognize that many key stakeholders may not have access to such resources and are committed to supporting participation in this issue wherever resources are a barrier. For more information about what support may be available, please visit OA funding and support, or email OAfundingpolicy@springernature.com or the Editor-in-Chief.
Publishing Model: Open Access
Deadline: Oct 14, 2026
Refining eating disorder-PTSD links: the dissociative subtype of PTSD (DPTSD) and complex PTSD (CPTSD)
Journal of Eating Disorders is calling for submissions to our Collection on Refining eating disorder-PTSD links: the dissociative subtype of PTSD (DPTSD) and complex PTSD (CPTSD).
Since the DSM-III description of posttraumatic stress disorder (PTSD) in 1980, a myriad of studies has substantiated the important role that traumatic events and posttraumatic stress have played in the predisposition, precipitation and perpetration of feeding and eating disorders. Integrated treatments that address both conditions and other trauma related comorbidities have become of major interest to the field, although much work remains to be done to develop and disseminate evidence-based strategies. In 2013, the DSM-5 added the dissociative subtype of PTSD, which is characterized by PTSD symptoms and depersonalization and/or derealization, and in 2022, the ICD-11 added complex PTSD to the diagnostic mix, which in addition to PTSD includes disturbances in self-organization. Each of these conditions has been shown to predict greater severity and more complex comorbidity, yet these syndromes are only beginning to be explored in relation to feeding and eating disorder psychopathology and phenomenology.
This Collection will focus on enhancing our understanding of these posttraumatic variations in relationship to feeding and eating disorders. Articles related to the epidemiology, phenomenology, psychoneurobiology, and treatment approaches for these specific PTSD subtypes are of particular relevance. In addition, articles that examine the commonalities and differences between classical PTSD, complex PTSD, and the dissociative subtype of PTSD in relation to feeding and eating disorders are of great interest.
This Collection is very much in alignment with many of the 17 goals proposed by the United Nations Department of Economic and Social Affairs, Sustainable Development. Those that are especially relevant goals that directly or indirectly influence the development of eating disorders and PTSD include “zero hunger,” “good health and well-being,” “quality education,” “gender equality,” “reduced inequalities,” “clean water and sanitation,” “sustainable cities and communities,” and “peace, justice and strong institutions.”
This Collection supports and amplifies research related to SDG 3, Good Health and Well-Being.
All submissions in this collection undergo the journal’s standard peer review process. Similarly, all manuscripts authored by a Guest Editor(s) will be handled by the Editor-in-Chief. As an open access publication, this journal levies an article processing fee (details here). We recognize that many key stakeholders may not have access to such resources and are committed to supporting participation in this issue wherever resources are a barrier. For more information about what support may be available, please visit OA funding and support, or email OAfundingpolicy@springernature.com or the Editor-in-Chief.
Publishing Model: Open Access
Deadline: Jun 01, 2026

Please sign in or register for FREE
If you are a registered user on Research Communities by Springer Nature, please sign in