Toward Precision Medicine Approaches to Facilitate Safer Opioid Treatment
Published in Healthcare & Nursing
“We as a profession have caused an epidemic that is bigger than the HIV epidemic....The cause in the opioid epidemic starts with getting a prescription of opioids from physicians”
- Atule Gawande
Scope of the prescription opioid problem
Over the last 10-15 years, opioid prescribing by healthcare providers has increasingly become recognized as a high-risk event. While the current illicit fentanyl crisis has changed the landscape, escalated the number of annual opioid-related deaths, and has in many ways overshadowed prescription opioid deaths, prescription opioids remain an important factor in the crisis. Their use can result in overdose (particularly when combined with other sedating drugs) and they serve as a precursor to illicit opioid use for some patients. In fact, the number of deaths from commonly prescribed opioids has not changed much since 20101 despite aggressive policy and regulatory efforts. Prescription opioids have thus become a double-edged sword -- they are a critical tool for humane provision of medical care (analgesia), but also create a pathway to opioid use disorder (OUD). In addition to the dangers of addiction, long term opioid use is also a contributor to the development of chronic pain. Not every person who receives a prescription for an opioid misuses the drug, develops dependence, or progresses to OUD; however, we currently are unable to identify patients at highest risk. This puts healthcare providers in a difficult position where they must carefully balance the desire (and duty) to alleviate suffering with the risk of long-term consequences of opioid use.
A novel precision medicine solution
Patients’ opioid use trajectories are unique and dependent on dynamic factors that cannot be easily assessed in routine clinical practice. Precision medicine approaches2 provide the opportunity to tailor prescribing to the individual based on risk; this is in stark contrast to one-size-fits all prescribing which misses opportunities to intervene or may lead to undertreatment of pain. Objective, continuous physiologic monitoring of opioid use provides an opportunity to employ this type of tailored approach. Preliminary data suggest both acceptability and feasibility3,4. An ideal digital diagnostic for opioid monitoring would be able to accurately and passively identify opioid use events, monitor for evidence of associated physiologic adaptations (such as opioid dependence and withdrawal), and deliver actionable insights to the clinician and patient. This could be coupled with a digital therapeutic to offer alternative pain management strategies and facilitate an opioid sparing approach before maladaptive patterns of opioid use occur. Physiologic responses to opioids are not straightforward: both acute responses to a single dose and sub-acute/chronic adaptations are impacted by a variety of individual and treatment factors. Acute physiologic effects of opioids are potentiated by sedating and cardiovascular drugs, and blunted by stimulants. Chronic adaptations are impacted by amount and duration of exposure, and genetics, among other factors. In order to achieve our goal of creating a digital diagnostic tool for opioid use monitoring, we must first understand how well we can detect opioid use, which confounders need to be accounted for in modeling strategies, and which are inconsequential.
Refining and Understanding the Digital Biomarker
In this paper, we explored the use of machine learning models applied to physiologic data collected by a wearable sensor (the Empatica E4, Figure 1) to detect opioid administrations. We also explored individual- and treatment-level factors that impacted model performance.
Figure 1: Empatica E4

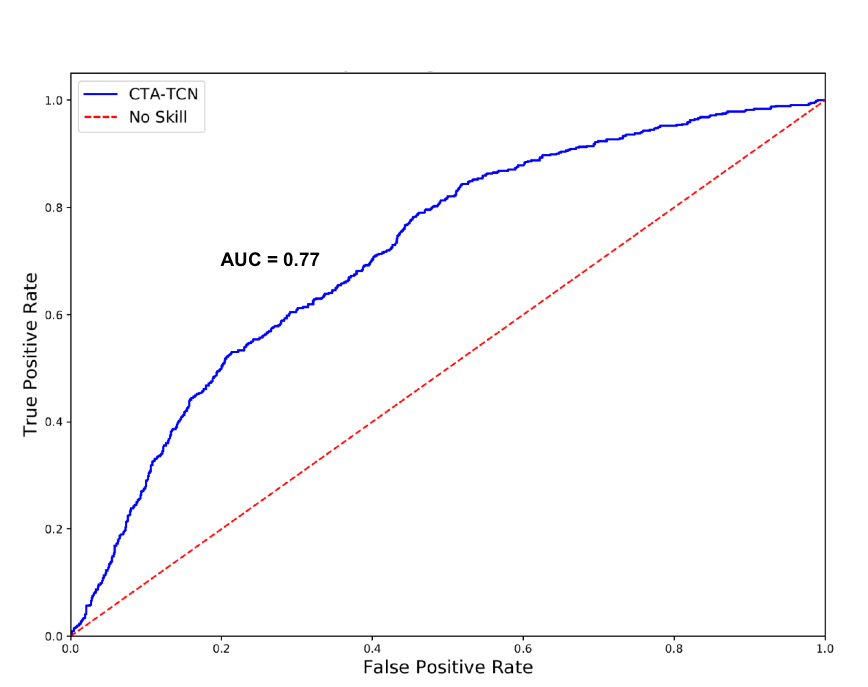
To achieve this goal, we collected over 2,000 hours of sensor data from 36 participants, including 339 discreet opioid-use events- defined as an in-hospital-intravenous opioid administration confirmed by both patient report and electronic health record documentation. To understand features that aid in opioid detection, we first explored sensor-based features that change after opioid administration. Reassuringly, these were generally consistent with known opioid physiology (decreases and overall slowing in motion, increases in skin temperature, and increases in heart rate variability). Next, we built machine leaning models to predict whether an opioid administration occurred in a given stream of sensor data, and if so, when. The best performing model was a Channel-Temporal Attention-Temporal Convolutional Network (CTA-TCN) model, which detected an opioid use event, on average, within 8.6 minutes of administration and with 77% specificity and 80% sensitivity.
Figure 2: ROC curve for CTA-TCN model
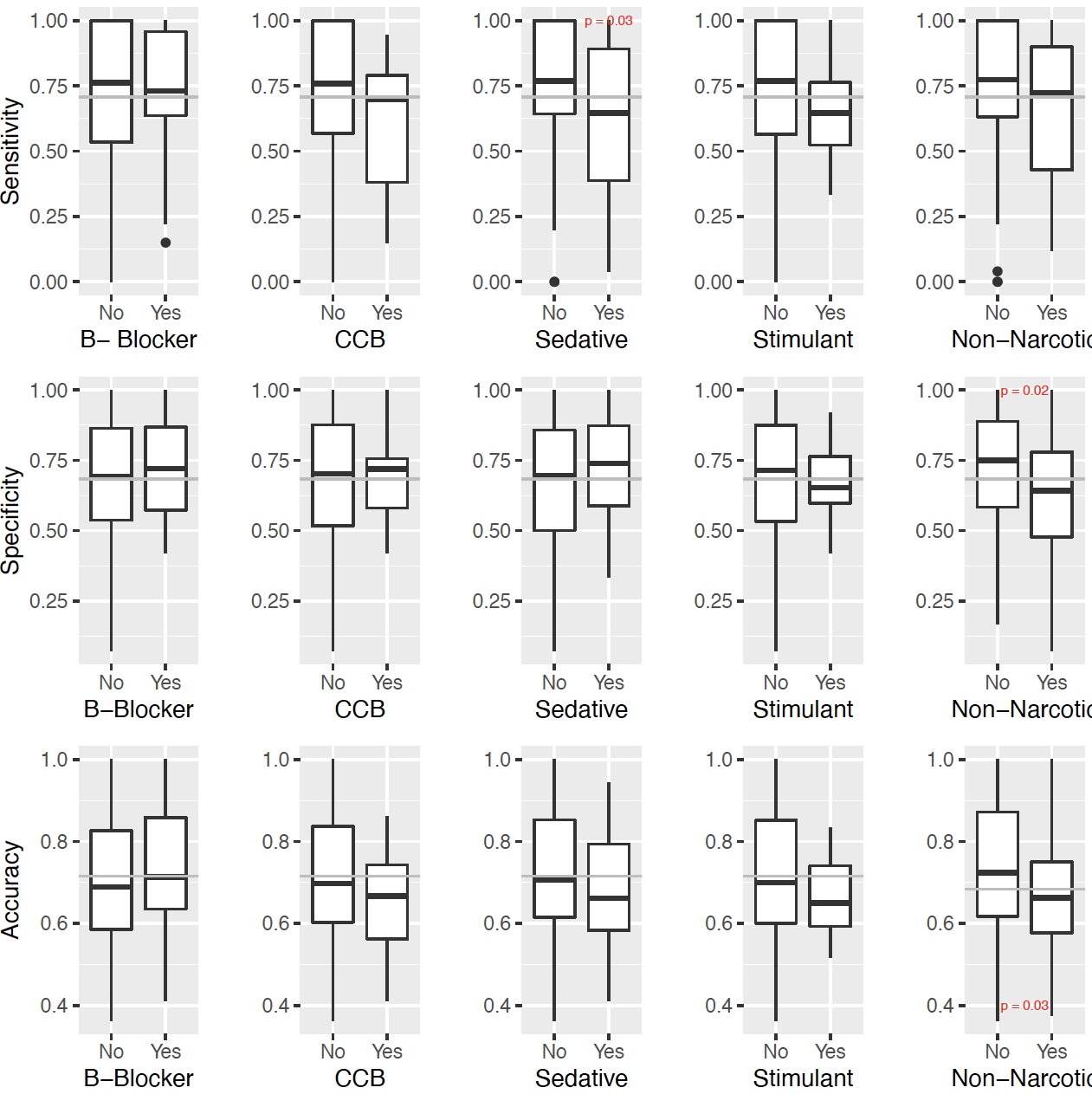
Finally, we evaluated the performance of the best model in a variety of subgroups based on patient factors (e.g., age, sex, medical history) and treatment factors (e.g., concomitant use of different medication classes). Most of the co-administered medications had little effect on model performance. Interestingly, co-administered non-opioid pain medications had a significant negative impact on model performance, raising questions about the contributions of pain to the detection of opioid effect.
Figure 3: Model metrics by co-administered medications
Leveraging Digital Biomarkers to Personalize Opioid Therapy
Once refined, these sensor-based signals can promote safer opioid use by leveraging gradual physiologic changes to identify patients at risk for complications of opioid therapy. Before this can be achieved however, they need to be validated in larger populations, made device agnostic, and correlated with clinical outcomes. Fully mature digital opioid pharmacovigilance strategies could completely shift the concepts of iatrogenic opioid dependence and OUD making them identifiable in early stages, and preventable. This would decrease the risks associated with opioid prescribing, allow for safe and personalized opioid pain management, and reduce mortality associated with prescription opioids.
References
- Centers for Disease Control and Prevention. Understanding the Epidemic 2021. Available from: https://www.cdc.gov/drugoverdose/epidemic/index.html.
- FDA. Precision Medicine. Available from: www.fda.gov/medical-devices/in-vitro-diagnostics/precision-medicine
- Carreiro, S., Chapman, B. P., Lucey, E., Boyer, E. W., Babu, K., & Smelson, D. (2022) Perceptions on Wearable Sensor-Based Interventions for Monitoring of Opioid Therapy. Frontiers in Digital Health, 212.
- Carreiro, S., Wittbold, K., Indic, P., Fang, H., Zhang, J., & Boyer, E. W. (2016). Wearable biosensors to detect physiologic change during opioid use. Journal of medical toxicology, 12(3), 255-262.
Follow the Topic
-
npj Digital Medicine
An online open-access journal dedicated to publishing research in all aspects of digital medicine, including the clinical application and implementation of digital and mobile technologies, virtual healthcare, and novel applications of artificial intelligence and informatics.
Related Collections
With Collections, you can get published faster and increase your visibility.
Artificial Intelligence in Sports Medicine
Publishing Model: Open Access
Deadline: Jul 21, 2026
Impact of Agentic AI on Care Delivery
Publishing Model: Open Access
Deadline: Jul 12, 2026



Please sign in or register for FREE
If you are a registered user on Research Communities by Springer Nature, please sign in