Deep Learning System to Predict the 5-year Risk of High Myopia using Fundus Imaging in Children
Published in Healthcare & Nursing
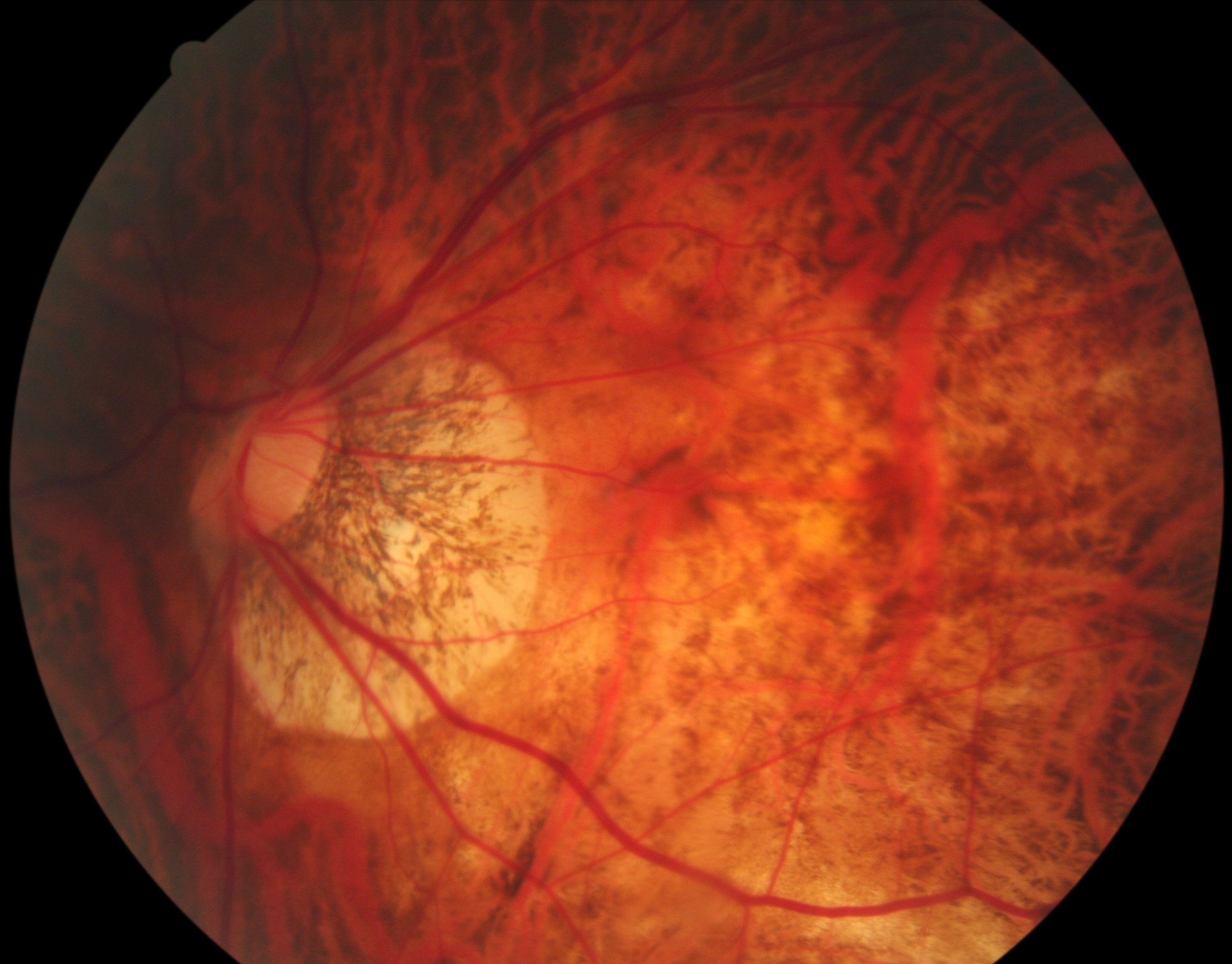
Current projections are alarming with half of the world’s entire population expected to be affected with myopia by the year 2050. This distribution is geographically dependent with higher prevalence seen in the Asian population. Widely referred to as the myopia capital of the world, Singapore’s unique physical and socioeconomic landscape has contributed to some of the highest levels of myopic prevalence seen globally. At present, approximately 20% of Singaporean children are myopic by the age of 7, with the prevalence exceeding 70-80% upon completion of tertiary education.
With increasing research and development, we now have the tools to prevent high myopia.These interventions include atropine eyedrops and optical devices (e.g., myopic defocus spectacles and multifocal contact lenses) that may reduce myopia progression in children. However, these treatments are not silver bullets and may not be suitable for all children. This is due to varying effectiveness for different age groups, logistic availability as well as potential side effects. A key area of research is to identify children who are ‘at risk’ of developing high myopia with greater precision, so that these interventions may be appropriately introduced to these children.
We aim to use simple, accessible and objective measures that are available during a single baseline visit to address the unmet need of identifying children at risk of developing high myopia. We developed a modular deep learning system based on single-time point objective data and fundus imaging to predict the 5-year development of high myopia in a multi-ethnic group of children aged between 6 to 12 years old at baseline.Our models demonstrated clinically acceptable predictive performance with Area under the ROC Curve (AUCs) ranging from 0.90 to 0.98. Importantly, the fundus image-only model demonstrated comparable performance (AUC = 0.94) against clinical models (AUC 0.90-0.97). Marginal benefit or decline in performance was noticed with additional 1 year follow-up progression data of SE.
The performance of our fundus image-only model has the potential to be translated and implemented into community or school-based programs to identify at-risk children for further assessment and intervention if required. Applying post-processing techniques to saliency heatmaps, generated using Integrated Gradient techniques, our models appropriately identified the disc and macular as areas of interest, consistent with areas of future myopic disc changes and myopic macular degeneration.
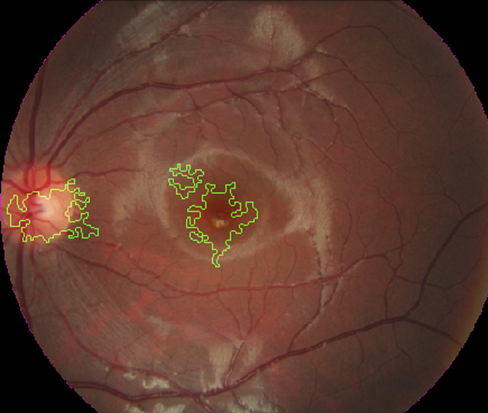
Our predictive deep learning system is designed to address specific clinical challenges, and with the most clinical impact. First, we have a target age group of children aged 6-12 years old who are most vulnerable to myopia progression and also amenable to myopia control therapies.Second, we used only objective inputs to avoid biases related to subjective recall – and these are obtained at one single time point (baseline), thereby eliminating the need for repeated, longitudinal follow-up before a clinical decision can be made and avoiding unnecessary delay of treatment for high-risk individuals. Third, our various image-based and mixed-clinical models produced clinically acceptable performances, allowing for implementation in various clinical settings with the availability of imaging systems. As a further enhancement, our system was trained and tested using a multi-ethnic population which improves the overall generalizability of the results. Fourth, our system delivered robust predictive performance against an external validation dataset which was dissimilar to the training datasets. This suggests that we could have the capacity to achieve good performance against unique external datasets, which would require substantiation through further validations.
In summary, we have developed a predictive deep learning system using a baseline fundus image and objective clinical data to identify schoolchildren at risk of developing high myopia later on in their teenage years. Through early identification, targeted and timely myopia control therapies may be instituted to reduce the risk of developing high myopia in these children. The fundus image-only model may be implemented via integration into fundus camera.
Follow the Topic
-
npj Digital Medicine
An online open-access journal dedicated to publishing research in all aspects of digital medicine, including the clinical application and implementation of digital and mobile technologies, virtual healthcare, and novel applications of artificial intelligence and informatics.
Related Collections
With Collections, you can get published faster and increase your visibility.
Evaluating the Real-World Clinical Performance of AI
Publishing Model: Open Access
Deadline: Jun 03, 2026
Impact of Agentic AI on Care Delivery
Publishing Model: Open Access
Deadline: Jul 12, 2026






Please sign in or register for FREE
If you are a registered user on Research Communities by Springer Nature, please sign in