Wake slow waves in focal human epilepsy impact network activity and cognition
Published in Neuroscience and Anatomy & Physiology
Several months ago, our group identified a typical electrophysiological signature of sleep, namely sleep slow waves, in intracranial recordings of patients with focal epilepsy. This caused us great surprise, because the patients were awake, and, in fact, they were performing a memory task.
Slow waves, as their name suggests, are deflections, in the electrophysiological signal, lasting less than a second. Their amplitude clearly exceeds background noise. Epileptic spikes are often immediately followed by a slow wave. In addition, slow wave activity can occur in damaged areas of brain. In contrast, the waves that we identified were isolated; they did not immediately follow a spike and were different from those that accompany brain injury.
Initial observations were achieved on a few subjects, but the finding was intriguing enough to undergo a systematic search across several patients and test whether these findings were reproducible.
Across 25 patients recorded at University College London Hospital and then across 115 patients recorded at 2 different and independent centres, using automated software, we were able to identify slow waves during wakefulness as a common phenomenon in people with epilepsy. Although they were much rarer than during sleep, they were systematically identified. At that stage, several questions came to our mind. Do these waves have anything in common with typical sleep slow waves? Do these waves occur only in patients with epilepsy? Do these waves occur only in the temporal lobe? Do these waves have any interaction with epileptic spikes?
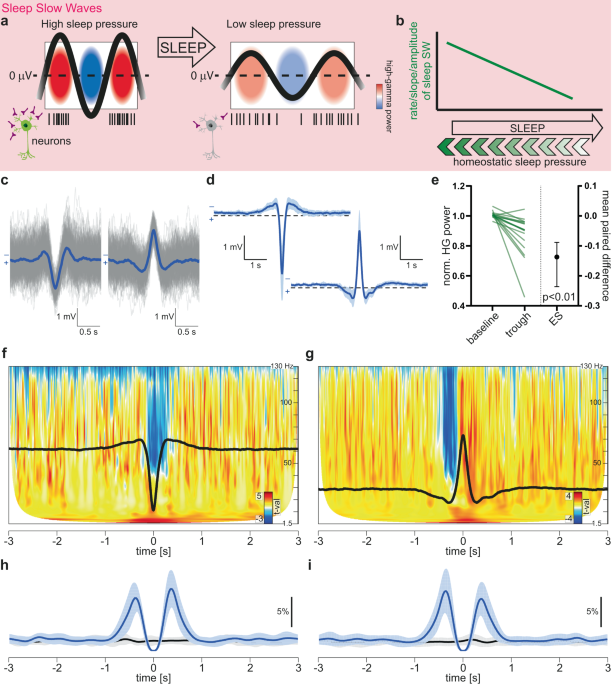
Up to now, slow waves were uniquely defined during sleep. Sleep-like slow waves had been observed in sleep-deprived rats 1 and in human subjects undergoing a cognitive task and complaining from attention lapses 2, but it was unknown whether typical slow waves with core features of sleep slow waves also occurred in humans during wakefulness. Hence, a first experiment that we undertook was to test whether the slow waves that we identified reproduced at least some of these core features, the main one being what is called a “neuronal down-state” 3. Sleep slow waves modulate neuronal discharges and imprint on their activity an alternation between high, synchronous activity (the “up-state”) and virtually absent activity (the “down-state”). Using micro-electrode recordings in humans, which allow to sample the activity of single neurons, we were able to confirm that slow waves of wakefulness, found in our recordings, were also associated with a down-state.
The structure of wake slow waves was thus very similar to that of sleep slow waves. What about their function?
The function of sleep slow waves is multiple, and probably not fully understood yet, but they have been involved in memory, clearance of the brain and restoration of a physiological state of excitability. Interestingly, sleep slow waves do not simply decrease excitability – they do it in a homeostatic loop. Indeed, their rate, amplitude and slope, which have been linked to their ability to decrease excitability, have also been shown to vary depending on the level of sleep-need, which can depend on the duration of the preceding awake period. The more slow waves are needed, the more they will provide a normalization of network excitability. Epilepsy is precisely a disease of excessive brain excitability. Hence, the next question that we raised regarding the function of wake slow waves was whether these waves, as sleep slow waves, were also involved in decreasing excitability, this time the increased excitability associated with epileptic activity, in a similar homeostatic loop.
To test the presence of a homeostatic loop, we needed to assess whether changes in background brain activity anticipate epileptic spikes and to which wake slow waves respond, as they would respond to increased excitability following a period of wakefulness. Then, to close the loop, we would need to test whether they provide negative feedback on the excitability associated with spikes.
In the first experiment, we tested whether the brain network becomes more excitable before a spike. As some evidence from the literature already suggested it, the finding of a similar increase in excitability before spikes in our data was not surprising. In the next experiment, we then tested whether slow waves respond to that increase in excitability. Although the rate of slow waves did not show evidence of change before epileptic spikes, their slope and amplitude increased progressively before epileptic spikes, as they would do after a period of wakefulness. In the third experiment, we wanted to test whether wake slow waves provide a negative feed-back on epileptic spikes.
The problem with this question… is to define its potential answers. Less prosaically, which outcome or readout should we select? Testing whether wake slow waves prevent the occurrence of epileptic spikes can be challenging, because testing the absence of an event is simply more difficult than testing its occurrence. We thus decided to test whether the proximity of an epileptic spike with a preceding slow wave is associated with a change in the excitability associated with that epileptic spike. Not only we found that this was the case, but the effect we calculated corresponded to approximately 1% of increase in excitability for each additional delay of 1 s since the last slow wave – this was quite remarkable.
If slow waves during wakefulness are protective, why are they so rare? Part of the answer might be that this restorative function of wake slow waves comes with a price. Since they impact significantly on neuronal activity (see the notion of “up-” and “down-state” above), we hypothesized that their presence would negatively impact on cognition. We tested this by calculating their rate in memory trials with correct and false answer, as well as in correlation with reaction time. While their presence did not affect accuracy, we observed that they were significantly more frequent when reaction time was prolonged. Hence, their rarity could be due, at least in part, to the fact that their presence inhibits normal brain processing. This hypothesis was raised in a high-profile review 4 and had been tested in the sleep-deprived rat 1.
Demonstrating causality in research on human subjects can be very challenging, because it would be necessary to manipulate brain activity. In our study, we show several converging evidence that slow waves could have a restorative effect on spikes, but so far, the evidence remains associative. Further works will show whether this is correct or if other parameters are involved in the process.
Altogether, our work paves the way for neurostimulation protocols that could take advantage of this intrinsic protective function against epileptic activity. The goal would be to accurately trigger or enhance slow waves in a manner that limits cognitive impact. Neurostimulation can be very efficient in certain diseases, such as Parkinson’s disease, but its efficacy in epilepsy remains limited. A better understanding of the underlying mechanism – as we propose here – could be crucial for refining the parameters of stimulation to optimize its impact.
References-
- Vyazovskiy, V. V. et al. Local sleep in awake rats. Nature 472, 443–447 (2011).
- Andrillon, T., Burns, A., Mackay, T., Windt, J. & Tsuchiya, N. Predicting lapses of attention with sleep-like slow waves. Nature Communications 12, (2021).
- Nir, Y. et al. Regional Slow Waves and Spindles in Human Sleep. Neuron 70, 153–169 (2011).
- Vyazovskiy, V. V. & Harris, K. D. Sleep and the single neuron: the role of global slow oscillations in individual cell rest. Nature Reviews Neuroscience 14, 443–451 (2013).
Follow the Topic
-
Nature Communications
An open access, multidisciplinary journal dedicated to publishing high-quality research in all areas of the biological, health, physical, chemical and Earth sciences.
Related Collections
With Collections, you can get published faster and increase your visibility.
Women's Health
Publishing Model: Hybrid
Deadline: Ongoing
Biosensing
Publishing Model: Hybrid
Deadline: Jun 30, 2026



Please sign in or register for FREE
If you are a registered user on Research Communities by Springer Nature, please sign in