DNA of neutrophil extracellular traps promote autoimmunity in chronic obstructive pulmonary disease
Published in General & Internal Medicine and Immunology
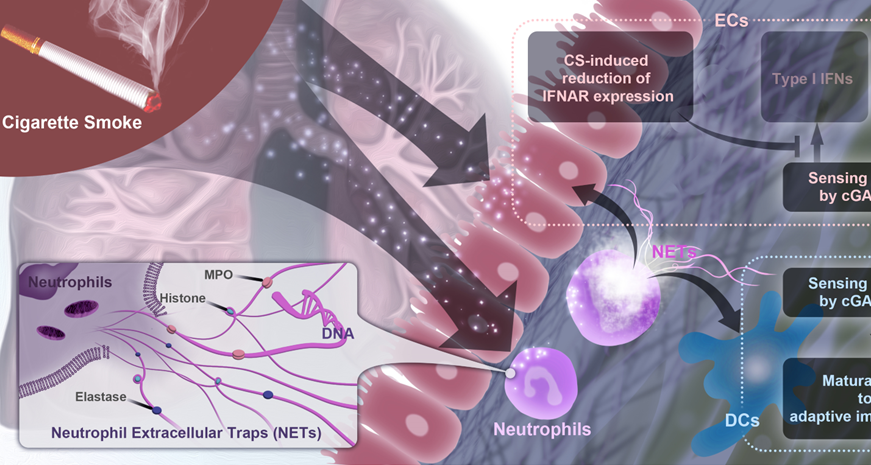
The “Why”
COPD is a leading cause of global morbidity and mortality. Airway inflammation assumes a pivotal and foundational role in the intricate pathogenetic mechanisms underlying COPD1. In contrast to the transient nature of acute airway inflammation induced by short-term exposure to cigarette smoke (CS), the airway inflammation observed in COPD sustained even after the cessation of cigarette smoking, thereby significantly contributing to airway damage, remodeling, loss of small airways and emphysema, and the consequential attenuation of current therapeutic interventions2,3.
However, the mechanisms underlying sustained airway inflammation have yet to be completely elucidated. Recently, researchers have suggested the involvement of neutrophil extracellular traps (NETs), a DNA framework that facilitates entrapping and eliminating pathogens, in the development of COPD: NETs levels in the induced sputum are associated with the severity of airflow limitation and the loss of microbiota diversity in patients with COPD4-6; in addition, NETs may participate in short-term CS-induced acute airway inflammation of mouse model by mediating the dysfunction of the airway epithelial cells (AECs) and dendritic cells (DCs)7-9. However, the following aspects remain unclear: (1) The contribution of NETs to persistent airway inflammation by initiating an autoimmune response in the long-term CS-induced COPD characterized by airflow limitation and emphysema; (2) The mechanisms behind cigarette smoke extract (CSE)-induced NETosis and the differences between the NETs derived from the neutrophils of patients with COPD and those of healthy individuals; (3) The role of NETs as therapeutic targets to control sustained airway inflammation in COPD.
Therefore, this study investigated whether and how NETs contribute to long-term CS-induced COPD, with a focus on the immunoregulatory effects of NETs-DNA on AECs, and the role of NETs and targeted pathways as therapeutic targets to alleviate persistent airway inflammation in COPD.
The “How”
This study validated its hypotheses through four key investigations (Fig. 1): (1) Investigating the mechanism and effect of Cigarette Smoke Extract (CSE) on neutrophil NETs release using freshly isolated human peripheral neutrophils; (2) Assessing NETs-DNA impacts on airway epithelial proliferation, NF-κB-mediated cytokine and Type-I IFN expressions-secretions, and dendritic cell maturation, elucidating cGAS and TLR9's crucial roles, via primary bronchial epithelial and monocyte-derived dendritic cells; (3) In a COPD murine model induced by chronic smoke exposure, evaluated CS-induced NETs' role in airway inflammation, employing cGAS−/− and TLR9−/− mice to block NETs-DNA sensing, mitoTEMPO to inhibit ROS-induced NETosis, and DNase-I for DNA degradation, with correlations to NF-κB inflammation and Type-I IFNs analyzed; (4) A COPD and control cohort study correlated key NETs components' (MPO, NE activity) alterations in Bronchoalveolar Lavage Fluid (BALF) with disease severity and NF-κB-related inflammatory mediator and Type-I IFN levels.
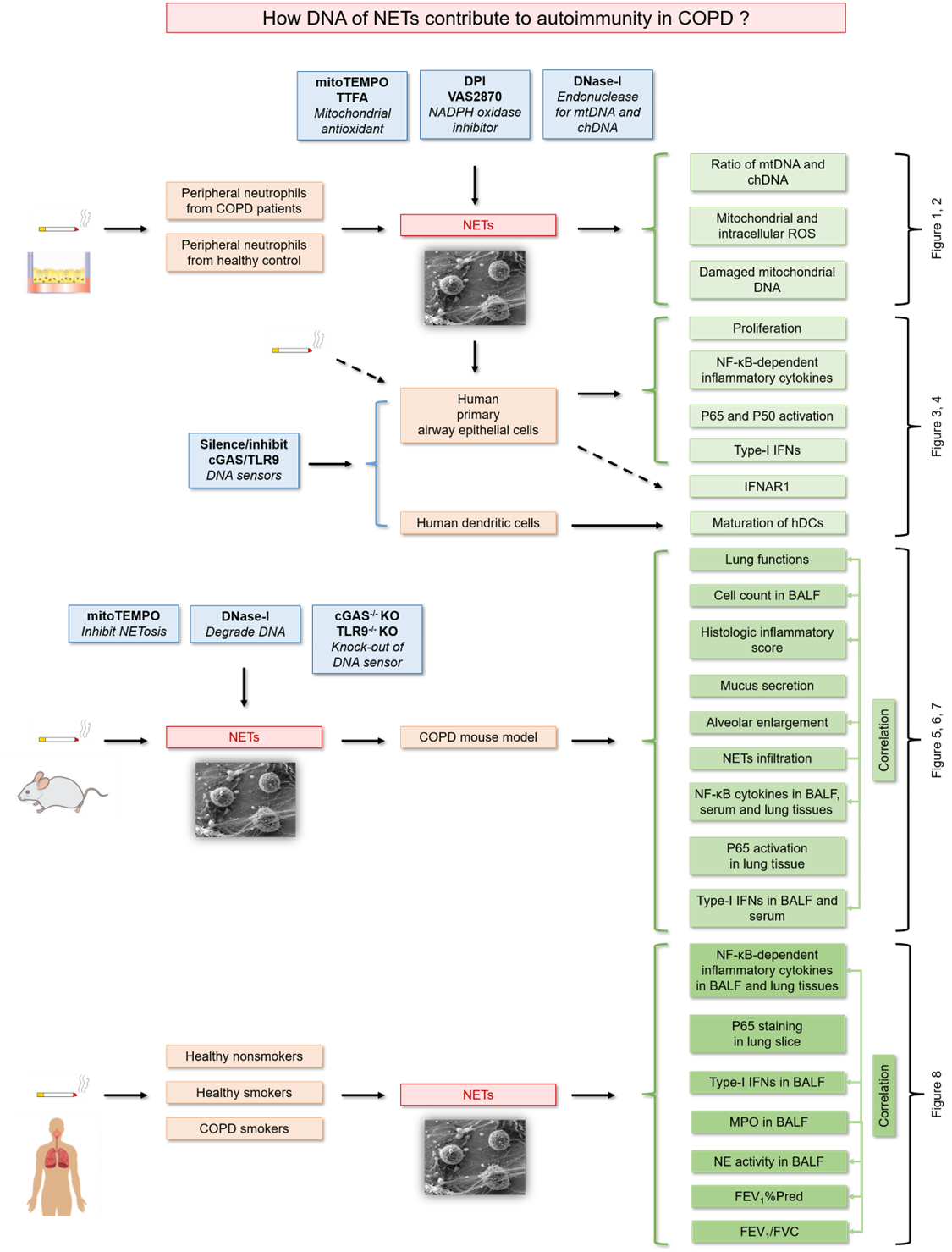
Figure 1. A schematic diagram displays the overall design of study.
The “What”
We revealed the immunomodulatory role of NETs in the long-term CS-induced COPD by providing the following evidence: (1) Neutrophils derived from patients with COPD displayed a stronger ability to release cigarette smoke extract (CSE)-induced NETs, which relied mainly on the mitochondrial respiratory chain; (2) NETs comprised high levels of oxidatively damaged mitochondrial DNA and nuclear/chromatinic DNA (NETs-DNA); (3) NETs-DNA stimulated the proliferation, the production of both nuclear factor kappa B (NF-κB)-dependent cytokines and type I interferons (IFNs) on human AECs, and the maturation of human DCs, which were ameliorated or reversed by the silencing or inhibition of two key DNA sensors, namely cyclic guanosine monophosphate-adenosine monophosphate synthase (cGAS) or toll-like receptor 9 (TLR9), respectively in vitro; (4) The in vivo blockage of NETs-DNA sensing using cGAS and TLR9 knockout mice, the inhibition of NETs formation by mitochondrial reactive oxygen species inhibitors (mitoTEMPO), and the degradation of NETs by DNase I resulted in reduced NETs infiltration, productions of NF-κB-dependent cytokines (but not Type I IFNs, due to an impaired expression of IFN-α/β receptor Subunit-1 by CS exposure), and alleviated airway inflammation, airflow limitation, and emphysema in a well-established long-term CS-induced COPD mouse model; (5) The severity of NETs infiltration was correlated with the severity of airway inflammation, and lung functions in CS-treated mice. Moreover, myeloperoxidase (a primary component of NETs) levels were correlated with those of NF-κB-dependent cytokines, but not those of type I IFNs, in the BALF of patients with COPD.
Take-home messages
Taken together, these results illustrated that the sensing of CS-induced NETs-DNA by cGAS and TLR9 in AECs and DCs promotes NF-κB (but not type I IFN)-dependent autoimmunity, which is essential for long-term CS-induced sustained airway inflammation in COPD (Fig. 2). This study shed light on the role of NETs in promoting autoimmune response to sustain the airway inflammation in COPD; Therefore, despite the role of NETs in eliminating invaded pathogens and maintaining microbiota diversity in the lungs, NETs may act as a double-edged sword in the pathogenies of COPD. These findings may extend our understanding of the autoimmune dysregulation in COPD and indicate that the NETs and the sensing receptors are potential therapeutic targets for the treatment of persistent airway inflammation in patients with COPD.
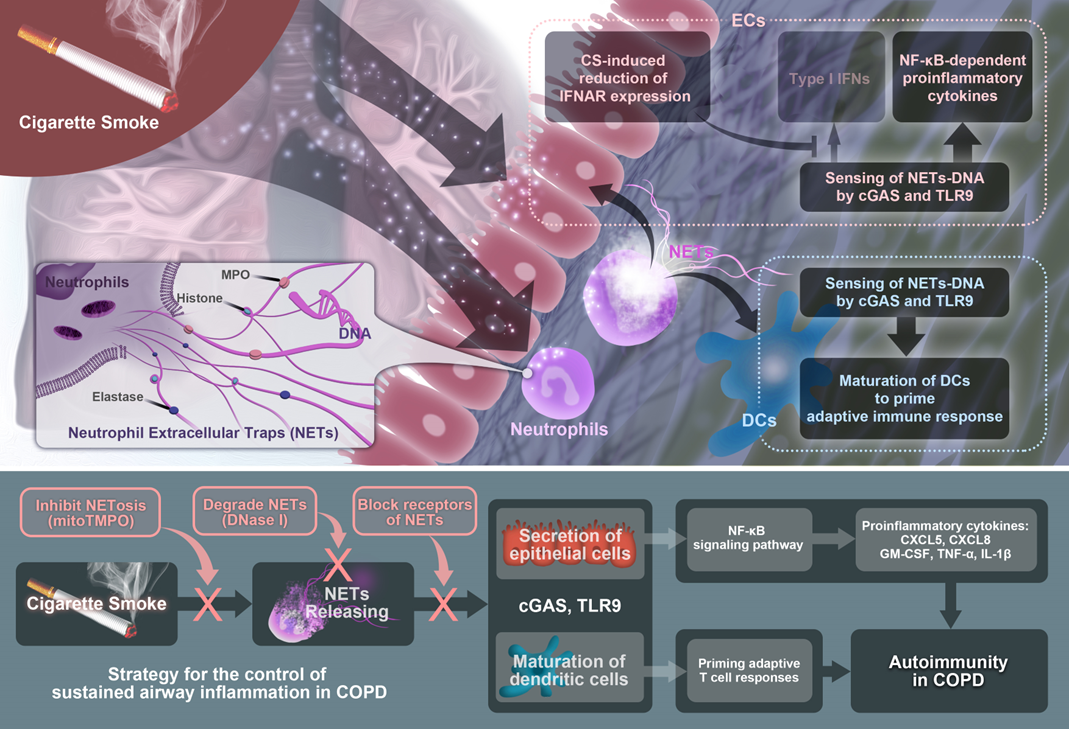
Figure 2. A schematic diagram displays the role of NETs in promoting autoimmune response by inducing aberrant production of NF-κB-dependent cytokines via cGAS and TLR9 to sustain the airway inflammation in COPD.
References
1 http://goldcopd.org/. Global Initiative for Chronic Obstructive Lung Disease (2024).
2 Hogg, J., Paré, P. & Hackett, T. The Contribution of Small Airway Obstruction to the Pathogenesis of Chronic Obstructive Pulmonary Disease. Physiol. Rev. 97, 529-552 (2017). https://doi.org:10.1152/physrev.00025.2015
3 Oelsner, E. et al. Lung function decline in former smokers and low-intensity current smokers: a secondary data analysis of the NHLBI Pooled Cohorts Study. Lancet Respir. Med. 8, 34-44 (2020). https://doi.org:10.1016/s2213-2600(19)30276-0
4 Grabcanovic-Musija, F. et al. Neutrophil extracellular trap (NET) formation characterises stable and exacerbated COPD and correlates with airflow limitation. Respir. Res. 16, 59 (2015). https://doi.org:10.1186/s12931-015-0221-7
5 Dicker, A. et al. Neutrophil extracellular traps are associated with disease severity and microbiota diversity in patients with chronic obstructive pulmonary disease. J. Allergy Clin. Immunol. 141, 117-127 (2018). https://doi.org:10.1016/j.jaci.2017.04.022
6 Wright, T. et al. Neutrophil extracellular traps are associated with inflammation in chronic airway disease. Respirology 21, 467-475 (2016). https://doi.org:10.1111/resp.12730
7 Zhang, H. et al. Erythromycin suppresses neutrophil extracellular traps in smoking-related chronic pulmonary inflammation. Cell Death Dis. 10, 678 (2019). https://doi.org:10.1038/s41419-019-1909-2
8 Zou, Y. et al. Neutrophil extracellular traps induced by cigarette smoke contribute to airway inflammation in mice. Exp. Cell. Res. 389, 111888 (2020). https://doi.org:10.1016/j.yexcr.2020.111888
9 Qiu, S. et al. Neutrophil extracellular traps induced by cigarette smoke activate plasmacytoid dendritic cells. Thorax 72, 1084-1093 (2017). https://doi.org:10.1136/thoraxjnl-2016-209887
Follow the Topic
-
Signal Transduction and Targeted Therapy
This is an international, peer-reviewed, open-access journal publishing articles related to signal transduction in physiological and pathological processes, alongside signal transduction-targeted therapeutics in the form of biological agents and small molecular drugs used to treat human diseases.





Please sign in or register for FREE
If you are a registered user on Research Communities by Springer Nature, please sign in