Engineering mini fatty livers for drug discovery
Published in Bioengineering & Biotechnology
Did you ever wonder if you suffer from fatty liver? Probably not, but maybe you should. Over a quarter of the worldwide population suffers from some form of non-alcoholic fatty liver disease, or in short NAFLD1. Worryingly, this seems to be only the tip of the iceberg as mathematical predictions point toward the possibility that over half of the adult population will be affected by 20402.
What is NAFLD exactly? It is an umbrella term for a complex disease spectrum that starts from the transformation of a healthy liver into a fatty liver, a.k.a. steatosis. A certain percentage of steatosis patients further progress to develop NASH (non-alcoholic steatohepatitis), a condition in which the liver becomes inflamed. NASH is often accompanied by the build-up of scar tissue in the liver (fibrosis). Upon too much and prolonged damage, the liver enters a state of cirrhosis, an irreversible end-stage disease that can lead to liver failure. NAFLD is a major risk factor for the development of liver cancer and it is also ranks among the top causes for the need of liver transplantation.
Well... how do we treat NAFLD? Currently, dietary and lifestyle interventions are the sole options to combat NAFLD, as there are no approved drugs for NAFLD. Such a prevalent disease and no drug therapies - how is this possible? As mentioned, the disease has risen with immense magnitude and speed. Model systems to grasp human NAFLD biology and to evaluate drugs remain extremely scarce. Mouse models differ greatly in their metabolism and as such their translational relevance is limited. A handful human-based in vitro models have been described but with limited versatility.
Clearly, novel models are needed to combat the NAFLD epidemic.
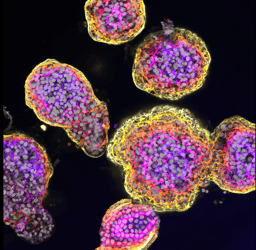
For the past few years, our research has focused on studying liver biology using 3D organoids from human hepatocytes3-4. These organoids can be long-term grown in culture while resembling many important features of the human liver. We established conditions under which we could robustly modify their genome, using different CRISPR-based approaches, enabling growing clonal gene-edited human hepatocyte organoid lines4-5.
Now, in our latest paper6, we joint the CRISPR forces with our human hepatocyte organoids to establish a versatile set of novel human fatty liver organoids. We show that these organoids allow to model different causes of steatosis, including diet-related causes ("Western diet-like") as well as genetic risk factors and monogenic lipid disorders.
Using the latest CRISPR tool, prime editing, we introduced the top associated risk variant (PNPLA3 I148M) into organoids that were originally wild type for the mutation. To our surprise, these mutant organoids spontaneously started to accumulate fat, and became much more fat when put under external fat loading. We were surprised that just having a single base variation could result in such drastic differences in the fatty liver phenotype. Knowing the science behind so well also made us aware of what could be currently going on in our very own bodies. We contemplated several times whether to pursue finding out if we are carriers of the mutation, but as of to date have not pulled the trigger... Would we need to adjust our diet, no more cheese or fast food? Obviously, we were jokingly discussing this and tended to get drawn away in these thoughts, but our organoid data are clear: genetic risk can dramatically impact on development of NAFLD.
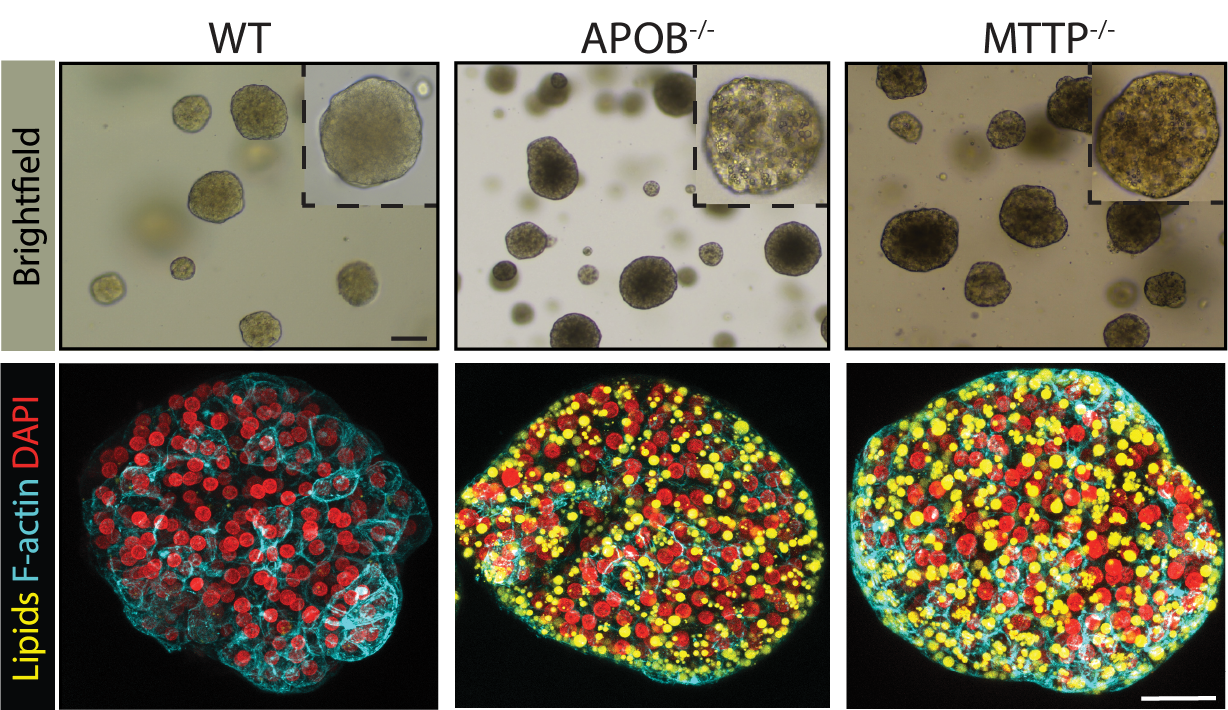
We also modeled two rare monogenetic lipid disorders (termed FHBL and ABL) that predispose to NAFLD, often already in pediatric patients. The effect of knocking out the causative genes (APOB or MTTP) was astonishing: the organoids developed spontaneous severe steatosis. We discovered that this was caused by the extensive accumulation of lipids that were originally generated from sugars.
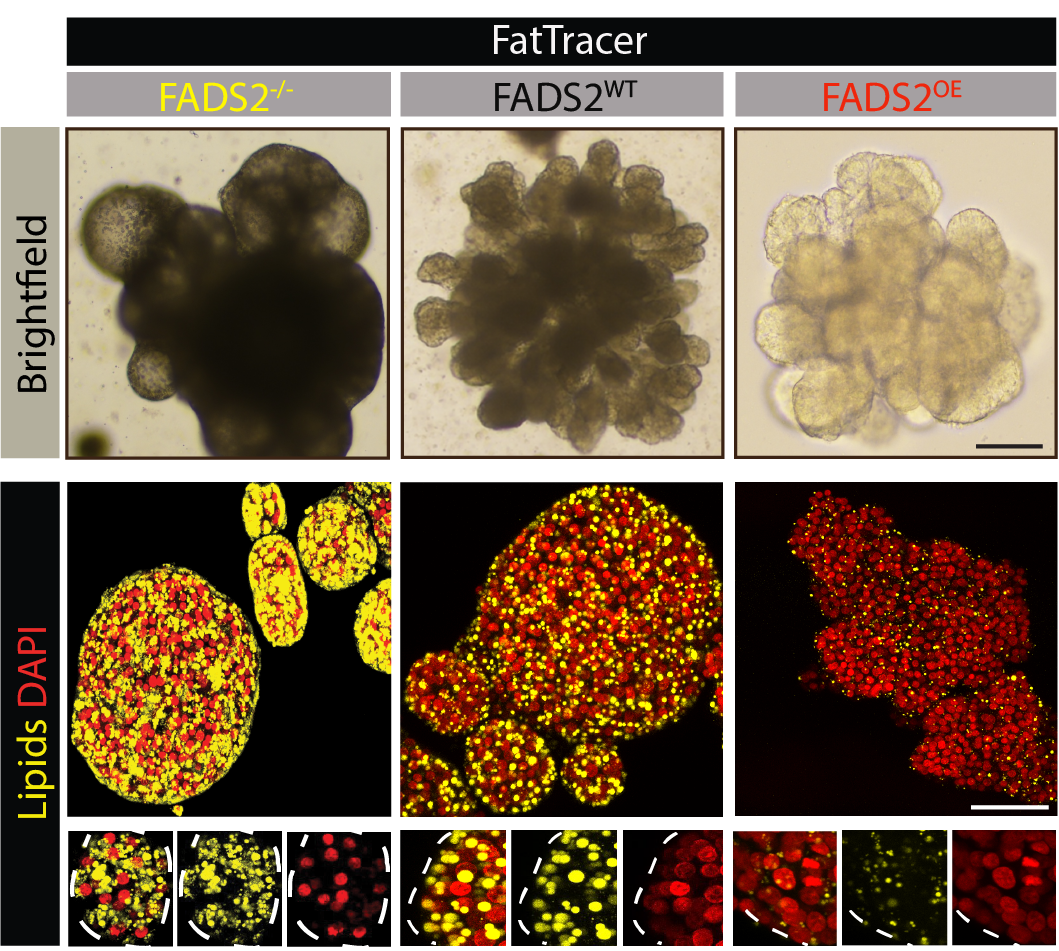
With our novel organoid models, we then proceeded to address two unmet needs in the field: 1) systematic and rapid drug screening and 2) establishing a genetic-based target screening system. Through drug screening we found out that a very specific set of drugs could effectively resolve steatosis, namely those that repress the synthesis of new fatty acids within the hepatocyte. We then turned the APOB- and MTTP-mutant organoids into a CRISPR-screening platform termed FatTracer. These mutant organoids were the perfect fit for such application for two simple reasons: they grew in culture as "natural" fatty livers and they could be further genome modified. FatTracer turned out to be a robust platform, where, in the span of a month, the effect of a specific gene knock-out on the fatty liver phenotype could be followed in real-time. Through screening 35 candidates, we discovered an important and novel role for FADS2 in steatosis biology. Loss of FADS2 aggravated steatosis, yet the opposite turned out to also work: increasing FADS2 expression could resolve steatosis, positioning FADS2 as an interesting candidate to further explore in the scope of NAFLD.
What's next? We envision that these novel human fatty liver organoid models will greatly facilitate large scale drug testing and genome-wide target discovery. At the same time, we are eager to explore their use to learn about the biology of NAFLD. As of yet, there are just so many questions that lack answers. Why are some individuals at heightened risk to develop fatty liver? Why do some people experience more rapid disease progression than others? Do we need to tailor treatment to each individual? We hope that our organoid models will aid in answering these questions in the near future.
References
1. Younossi, Z.M., Golabi, P., Paik, J.M. et al. The global epidemiology of nonalcoholic fatty liver disease (NAFLD) and nonalcoholic steatohepatitis (NASH): a systematic review. (2023) Hepatology.
2. Le, H., Yeo, Y.H., Zou, B. et al. Forecasted 2040 global prevalence of nonalcoholic fatty liver disease using hierarchical bayesian approach. Clin Mol Hepatol. 28(4):841-850.
3. Hu, H., Gehart, H., Artegiani, B. et al. Long-term expansion of functional mouse and human hepatocytes as 3D organoids. (2018) Cell 175(6):1591-1606.e19.
4. Hendriks, D.*#, Artegiani, B.*#, Hu, H. et al. Establishment of human fetal hepatocyte organoids and CRISPR-Cas9 based gene knock-in and knock-out in organoid cultures from human liver. (2021) Nat Protoc. 16(1):182-217.
5. Artegiani, B.*, Hendriks, D.*, Beumer, J. et al. Fast and efficient generation of knock-in human organoids using homology-independent CRISPR-Cas9 precision genome editing. (2020) Nat Cell Biol. 22(3):321-31.
6. Hendriks, D.#, ..., Artegiani, B.#, Clevers, H.#. Engineered human hepatocyte organoids enable CRISPR-based target discovery and drug screening for steatosis. (2023) Nat Biotechnol. https://www.nature.com/articles/s41587-023-01680-4
Follow the Topic
-
Nature Biotechnology
A monthly journal covering the science and business of biotechnology, with new concepts in technology/methodology of relevance to the biological, biomedical, agricultural and environmental sciences.


Please sign in or register for FREE
If you are a registered user on Research Communities by Springer Nature, please sign in