Fatal and non-fatal breast cancers in women targeted by BreastScreen Norway
Published in Cancer, Computational Sciences, and Public Health

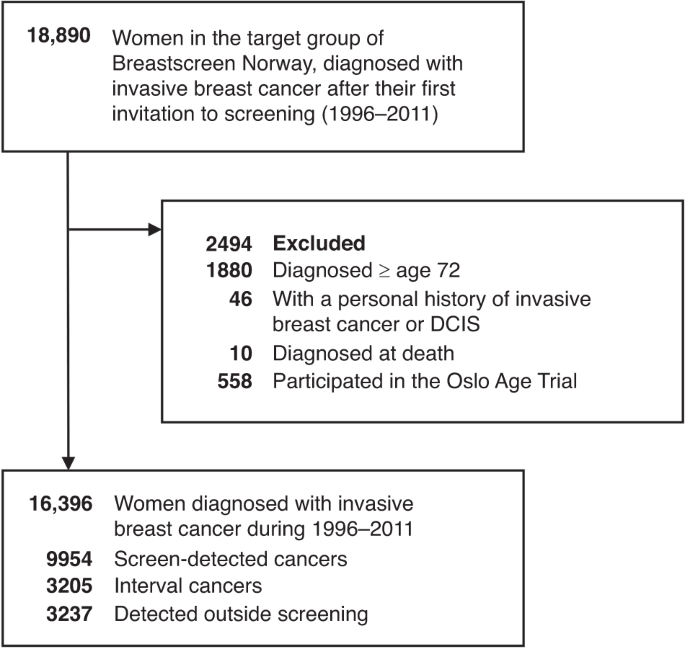
Organized screening with mammography aims to detect breast cancer in an early stage and thereby reduce deaths from this disease. In Norway, all women aged 50–69 are invited to screening every other year through BreastScreen Norway and 75% of invited women participate each year. The probability of surviving a diagnosis of breast cancer in Norway is 87% after ten years and is even higher for those whose cancer is detected at an early stage.

It is well established that screening with mammography reduces breast cancer deaths and there is a wealth of knowledge about a woman’s prognosis based on the histopathological characteristics of her disease. Nonetheless, less research has explored how women’s personal screening history plays a role in their prognosis and many breast cancer survivors experience anxiety related to dying from their disease.
Our study aimed to describe the tumour- and survival profiles of fatal and non-fatal breast cancers separately for those who attended and did not attend BreastScreen Norway after their last invitation. We considered a 10-year horizon when defining fatal and non-fatal cancers.
Making the most of artificial intelligence
We used a machine learning method called recursive partitioning to identify the tumour profiles associated with fatal and non-fatal breast cancers separately for those who attended or did not attend screening. Machine learning algorithms are typically used in a predictive setting where they are trained on large datasets and testing and validation is done using separate, independent datasets. In this context, such algorithms aim to make valid predictions from data that they have not been exposed to. In our study, we did not use machine learning to make predictions, but rather to describe our data. This is not a commonly used approach, but by training the machine learning algorithm on our whole dataset, we could use its output to describe different patterns in our data that might have been hard to identify using other approaches.
Opening the black box
We made several study design choices to help demonstrate the validity of our approach to clinicians, epidemiologists, policy makers, and others who are not data scientists by training. The most important design choice we made was to select a closed cohort where all study subjects had 10-years of follow-up. This ensured that our estimates for breast cancer survival were highly comparable to the proportion of women who did not die from their disease. This was important for us as authors because we wanted to demonstrate that this seemingly complex method could provide straightforward information that readers could verify themselves.
Many women have an excellent prognosis
The recursive partitioning algorithm identified different tumour profiles based on the associated survival outcomes for women who attended and did not attend screening. The algorithm selected well-known prognostic tumour characteristics to define these different groups. Overall, approximately half of women diagnosed with breast cancer in our study were identified as having breast cancer with a tumour profile associated with excellent (95–96%) 10-year breast cancer-specific survival. All of these women had attended BreastScreen Norway after their last invitation to screening. Although those who did not attend screening had poorer survival outcomes, there was also a group of women who hadn’t attended their last invitation to BreastScreen Norway who had over 90% 10-year breast cancer-specific survival – these women had small tumours that were likely diagnosed at a more curable stage than other women with cancer detected outside of the screening program.
Where do we go from here?
The recursive partitioning algorithm we used has several limitations, including that small changes in the data can result in different variables used to identify different tumour profiles. Additionally, to ensure that all women had 10 years of follow-up, we could only include cancer cases diagnosed before 2011 but these women do not necessarily represent the women being diagnosed with breast cancer today. However, these limitations improved the interpretability of our study results, which was important for us.
BreastScreen Norway and the Cancer Registry of Norway have substantial data holdings about breast cancer screening, diagnosis, treatment, and long-term outcomes that can, and should, be used to generate more knowledge about this disease. Future studies can build on the methodology presented in our paper by applying more robust methods to a contemporary cohort of women diagnosed with breast cancer. Although these methodological improvements would give results that cannot be easily checked with simple summary statistics, we hope that our study can act as a proof of concept to help non-data scientists better understand and trust results from machine learning methods. Overall, the results of our descriptive study demonstrated that women diagnosed with cancer after participating in BreastScreen Norway had better outcomes than those who did not attend. We hope clinicians may use the results of this study to inform and potentially reassure women diagnosed with breast cancer about potential 10-year outcomes.
Follow the Topic
-
British Journal of Cancer
This journal is devoted to publishing cutting edge discovery, translational and clinical cancer research across the broad spectrum of oncology.





Please sign in or register for FREE
If you are a registered user on Research Communities by Springer Nature, please sign in