From Lab to Live Demonstration: Testing an Eye-Tracking Tool for Autism in Real-World Settings
Published in Neuroscience, Biomedical Research, and General & Internal Medicine
The Story Behind the Paper
This paper began outside the laboratory.
For years, our team has worked on developing and validating an eye-tracking paradigm designed to provide an objective measure of social attention differences in Autism Spectrum Disorder (ASD). Clinical validation is essential, and our previous work demonstrated strong reliability and diagnostic performance in structured research settings. But we kept asking ourselves an important question:
Would this technology work in the real world — outside controlled laboratory environments?
A screening tool is only meaningful if it can function beyond ideal research conditions. It must work in busy, unpredictable environments, across cultures, languages, and diverse populations.
The opportunity to test this came unexpectedly.
During major international conferences in Qatar, Dubai, and the United States — including Arab Health, Web Summit, and INSAR — we showcased the device publicly. These were not clinical trials. They were live demonstrations at high-traffic events attended by healthcare professionals, researchers, technologists, entrepreneurs, and members of the general public.
Participation was voluntary and anonymous. Visitors approached out of curiosity and interest.
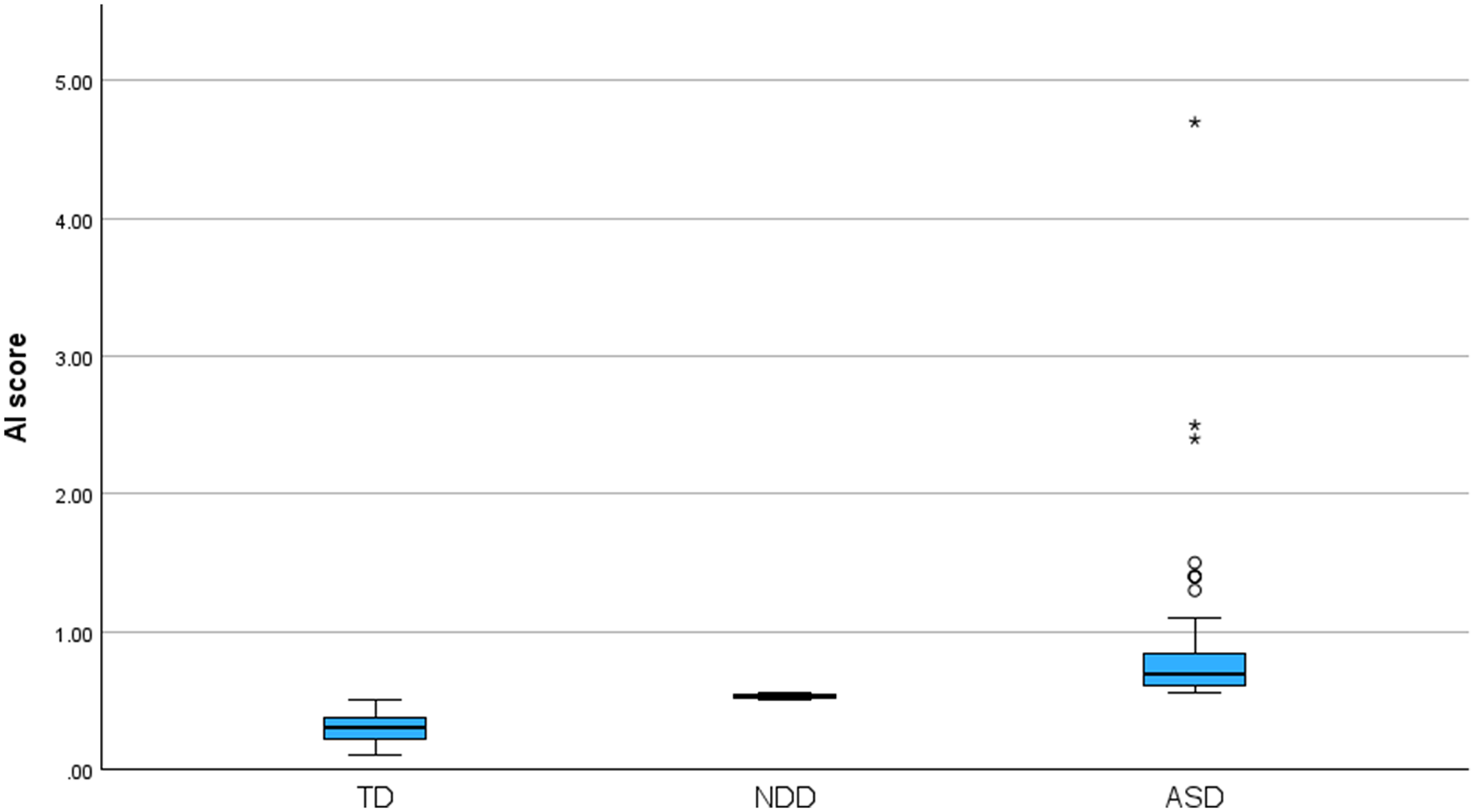
The eye-tracking assessment itself takes less than four minutes to complete. Participants view a series of social and non-social stimuli while the system records gaze patterns. From this, we compute a continuous measure known as the Autism Index (AI), which reflects social attention tendencies.
What started as a demonstration quickly became something more meaningful.
Over 500 adults engaged with the system across the three events. Despite the noise, lighting variability, time constraints, and dynamic nature of conference settings, the results were remarkably consistent.
The Autism Index clearly differentiated between typically developing individuals, neurodivergent individuals, and those classified as ASD-positive. Diagnostic performance remained exceptionally strong, even outside the laboratory.
Most notably, 95% of participants classified as ASD by the system reported having a prior formal diagnosis. This provided important reassurance that the tool was performing as expected — not only in controlled research settings, but in real-world environments.
Beyond the statistics, however, what stood out most was the human response.
Many participants were fascinated by the idea that something as natural as eye gaze could be measured objectively and translated into meaningful insight. Some individuals who screened positive shared that they had previously been advised to seek evaluation but had not yet pursued a formal assessment. These interactions highlighted the potential role of objective screening tools in supporting earlier identification and reducing uncertainty.
Traditional diagnostic pathways for ASD rely heavily on behavioral observation and clinician expertise. These methods are essential and remain the gold standard. However, they can be time-intensive and require specialized training. Eye-tracking does not aim to replace clinical assessment, but rather to complement it by providing rapid, objective data.
The fact that this entire screening paradigm can be completed in under four minutes makes it particularly promising for scalable applications. Its brevity, portability, and minimal burden suggest potential utility in broader screening contexts, including community and public-facing environments.
This experience reinforced something important for us as researchers: innovation must leave the lab.
A tool that performs well under ideal conditions must also prove itself in real-world settings. It must tolerate variability. It must function across cultures. It must remain robust outside carefully controlled environments.
This paper captures that transitional moment — the movement from validated research tool to practical, real-world deployment.
It represents an early but meaningful step toward making objective, accessible screening technologies more widely available and reducing barriers to autism identification globally.
Scientific progress does not end with validation. It continues through translation, application, and real-world testing.
For us, this study marked that next step.
Read the full article here: https://doi.org/10.1186/s12888-026-07840-5
Follow the Topic
-
BMC Psychiatry
This is an open access, peer-reviewed journal that encompasses a wide range of topics, including psychopharmacology, psychotherapy, and psychosocial approaches to psychiatric disorders, as well as genetics, pathophysiology, and epidemiology research.
Related Collections
With Collections, you can get published faster and increase your visibility.
Quality of life and recovery in schizophrenia
BMC Psychiatry is calling for submissions to our Quality of life and recovery in schizophrenia Collection. Beyond symptom control, enhancing quality of life and supporting meaningful recovery have become central goals of contemporary psychiatric care. This Collection aims to advance research that examines how clinical, social, and therapeutic factors influence quality of life and recovery in individuals diagnosed with schizophrenia and related spectrum disorders. We welcome contributions that move beyond symptom reduction to address functional outcomes, personal recovery, and sustained well-being across the lifespan.
Topics of interest include, but are not limited to:
- Determinants and measurement of quality of life in schizophrenia and schizoaffective disorder
- Clinical recovery versus personal recovery: conceptual models and outcome assessment
- Impact of positive, negative, and cognitive symptoms on overall functioning and social engagement
- Effects of antipsychotic treatments, long-acting injectable formulations, and adjunctive therapies on quality of life
- Psychosocial and community-based interventions supporting recovery, independence, and social inclusion
- Early intervention, duration of untreated psychosis, and long-term recovery trajectories
- Physical health comorbidities, premature mortality, and their influence on overall well-being
- Health system factors, stigma, and barriers to recovery-oriented care
- Patient-reported outcomes as complementary measures of recovery and subjective well-being
- Shared decision-making and patient engagement in recovery-oriented treatment planning
- Pharmacological optimization strategies and their impact on quality of life and everyday functioning
We invite original research that deepens understanding of how recovery and quality of life can be effectively promoted in schizophrenia. By integrating clinical evidence with patient-centered outcomes, this Collection seeks to inform practice, guide policy, and improve the lived experience of individuals affected by this disorder.
All manuscripts submitted to this journal, including those submitted to collections and special issues, are assessed in line with our editorial policies and the journal’s peer review process. Reviewers and editors are required to declare competing interests and can be excluded from the peer review process if a competing interest exists.
This Collection supports and amplifies research related to SDG 3: Good Health and Well-being and SDG 10: Reduced Inequalities.
Publishing Model: Open Access
Deadline: Nov 18, 2026
Alcohol use and psychiatric disorders
BMC Psychiatry is calling for submissions to our Collection on Alcohol use and psychiatric disorders. Alcohol use remains a leading contributor to global morbidity and mortality and is frequently associated with a wide range of psychiatric disorders, complicating diagnosis, treatment, and long-term outcomes. The co-occurrence of alcohol-related problems and psychiatric conditions poses significant challenges for patients, clinicians, and health systems alike.
This Collection aims to advance understanding of the relationship between alcohol use and psychiatric disorders across the lifespan. We welcome contributions that address underlying mechanisms, clinical presentations, and integrated approaches to assessment and treatment in both acute and long-term care settings.
Topics of interest include, but are not limited to:
- Epidemiology and patterns of comorbidity between alcohol use disorder and psychiatric diagnoses
- Alcohol use disorder in the context of major depressive disorder, anxiety disorders, bipolar disorder, schizophrenia, and trauma-related disorders
- Diagnostic challenges, including symptom overlap, masking effects, and differential diagnosis
- Neurobiological and genetic factors contributing to co-occurring alcohol use and psychiatric disorders
- Pharmacological and psychosocial treatment strategies, including relapse prevention and management of withdrawal
- The impact of alcohol use on treatment response, adherence, and prognosis in psychiatric populations
- Suicide risk, self-harm, and behavioral dysregulation associated with alcohol use and psychiatric illness
- Developmental and lifespan perspectives on alcohol use and psychiatric comorbidity, including adolescence and young adulthood
- Health disparities, stigma, and barriers to accessing integrated addiction and psychiatric care
We invite original research exploring how alcohol use interacts with psychiatric disorders and how care can be optimized for affected individuals. By integrating evidence from clinical practice, epidemiology, and health services research, this Collection seeks to inform effective, compassionate, and coordinated models of care.
All manuscripts submitted to this journal, including those submitted to collections and special issues, are assessed in line with our editorial policies and the journal’s peer review process. Reviewers and editors are required to declare competing interests and can be excluded from the peer review process if a competing interest exists.
This Collection supports and amplifies research related to SDG 3: Good Health and Well-Being.
Publishing Model: Open Access
Deadline: Dec 11, 2026


Please sign in or register for FREE
If you are a registered user on Research Communities by Springer Nature, please sign in