Impact of educational intervention on knowledge of antimicrobial resistance and antibiotic use patterns among healthcare students: a pre- and post-intervention study
Published in Microbiology
Methods
A quasi-experimental pre-and-post study design was conducted with unpaired groups of healthcare students. An educational intervention was carried out comprising of two 20-minute PowerPoint lectures, as well as question and answer sessions focused on understanding the spread, impact, and prevention of AMR. A self-administered questionnaire was given as a pre-test and repeated as a post-test immediately after the training. Students’ knowledge of AMR and patterns of antibiotic use was assessed pre-intervention while knowledge of AMR was assessed post-intervention. The knowledge was categorised into domains (Understanding Antibiotic and Antimicrobial Resistance; Spread and Impact of Antibiotic/Antimicrobial Resistance; Prevention of Antibiotic/Antimicrobial Resistance). The total score for each domain of knowledge tested was categorized into good knowledge (≥ 80%) and poor knowledge (< 80%).
Results
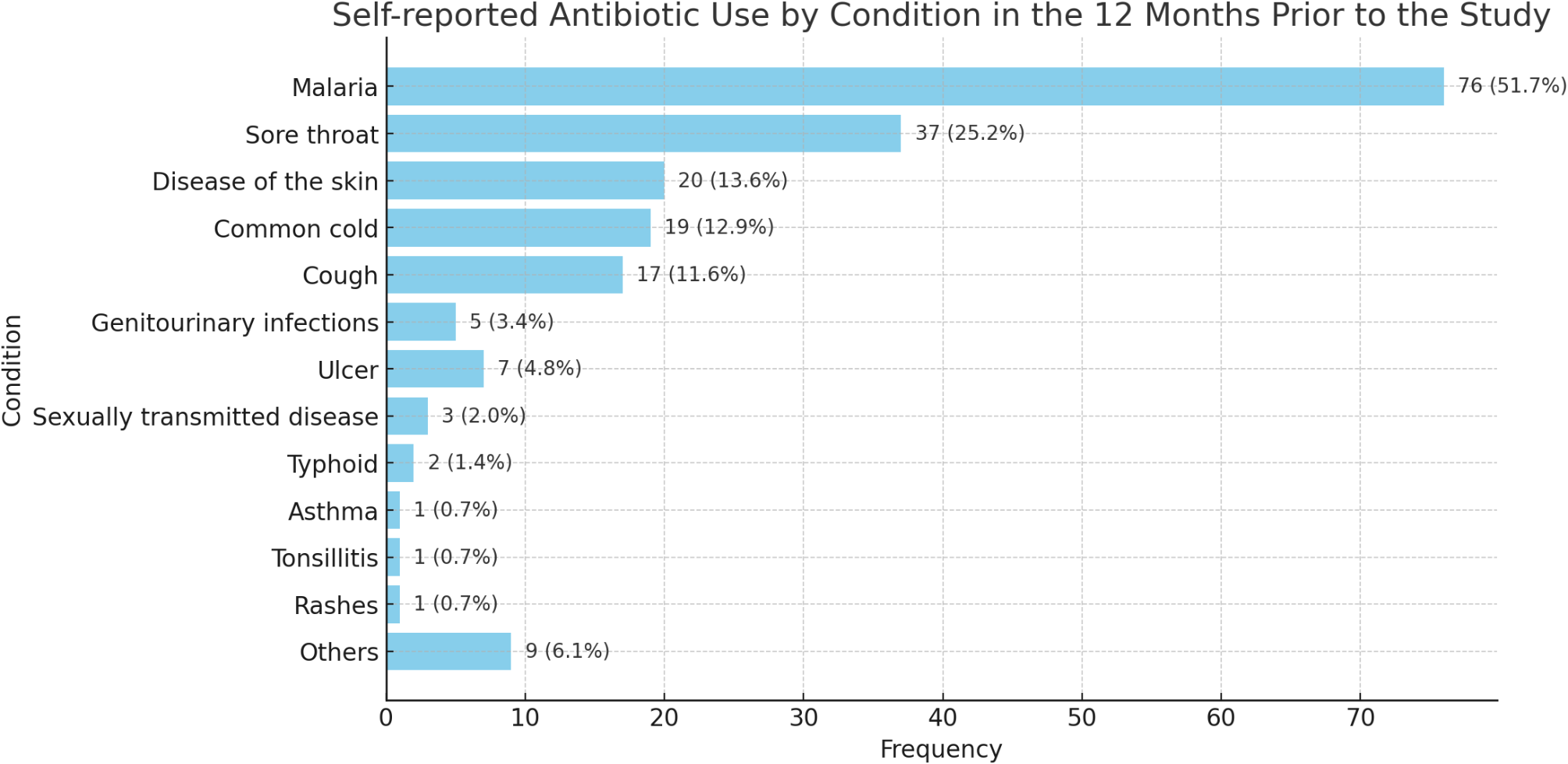
The number of participants in the pre- and post-intervention were 185 and 157 students with average age of 17.7 years and 17.8 years respectively. Post-intervention, there was a significant increase in students’ AMR knowledge, with correct responses regarding spread and impact of AMR increasing from 40.5% pre-intervention to 62.4% post-intervention (p < 0.001; φ (effect size = 0.218). The proportion of students demonstrating good overall knowledge increased from 28.1 to 44.6% (p = 0.001; φ (effect size = 0.171). Misconceptions, such as misunderstanding that antibiotic resistance does not result from the body becoming resistant to antibiotics, persisted but not statistically significant (24.9–17.2%, p = 0.055). Pre-intervention also revealed varied antibiotic use patterns, including the inappropriate use of antibiotics for malaria (51.7%, (n = 76)), and common cold (25.2% (n = 37)).
Conclusions
The study findings indicate that educational interventions can effectively improve healthcare students’ knowledge of AMR, though persistent misconceptions underscore the need for more targeted educational efforts. Incorporating structured AMR content into healthcare curricula could help the students contribute to antimicrobial stewardship. Future research should evaluate knowledge retention and behaviour changes to optimize the long-term impact of AMR education.
Follow the Topic
-
BMC Medical Education
This is an open access journal publishing original peer-reviewed research articles in relation to the education and training of healthcare professionals. It welcomes studies on students and professionals across all levels of education; education delivery aspects; and other education-related topics.
Related Collections
With Collections, you can get published faster and increase your visibility.
Transnational medical education programs
BMC Medical Education is calling for submissions to our Collection on Transnational medical education programs. As medical education expands beyond national boundaries, new opportunities and challenges are emerging in how curricula are delivered, quality is assured, and learners are supported across diverse cultural and institutional contexts. These cross-border educational partnerships are reshaping the way we define standards, prepare future health professionals, and foster global health equity.
This Collection invites research that critically examines the structure, outcomes, and implications of educational initiatives that operate across borders. Whether through institutional partnerships, dual-degree programs, offshore campuses, or digital learning platforms serving international student populations, transnational initiatives demand thoughtful attention to pedagogical alignment, accreditation, faculty development, and learner experience. We welcome insights that address the complexity of delivering medical education in settings where geographic, regulatory, and cultural contexts differ.
We encourage submissions on topics such as:
• Curriculum design and adaptation across cultural and regulatory contexts
• Accreditation and quality assurance in cross-border medical education
• Faculty development and support in international teaching environments
• Student experiences, identity formation, and transitions between institutions
• Governance models and institutional partnerships in global medical education
• Ethical considerations and power dynamics in transnational collaborations
• Role of digital platforms and technology-enhanced education in delivering cross-border education
This Collection aims to showcase diverse voices and evidence-based approaches that inform the development and sustainability of cross-national medical education programs. By fostering open dialogue and rigorous inquiry, we seek to support inclusive, high-quality education that prepares graduates to meet health needs across a global landscape.
All manuscripts submitted to this journal, including those submitted to collections and special issues, are assessed in line with our editorial policies and the journal’s peer review process. Reviewers and editors are required to declare competing interests and can be excluded from the peer review process if a competing interest exists.
This Collection supports and amplifies research related to SDG 3: Good Health and Well-being, SDG 4: Quality Education, and SDG 17: Partnerships for the Goals.
Publishing Model: Open Access
Deadline: Jun 23, 2026
Lifelong learning and patient safety
BMC Medical Education is calling for submissions to our Collection, Lifelong learning and patient safety. As healthcare delivery becomes increasingly complex, shaped by biomedical advances, digital transformation, demographic shifts, and changing patient expectations, so does the potential for errors and adverse events. This phenomenon makes it essential to equip all healthcare professionals with training and tools to prioritize patient safety across different clinical environments.
Patient safety is a global health priority, with the World Health Organization identifying unsafe care as one of the leading causes of avoidable morbidity and mortality worldwide. While traditional models of competence, validated at a single point in time through licensure or certification, can be valuable, addressing this challenge requires a workforce that is continuously learning, adaptive, and equipped to respond to evolving patient safety threats. Lifelong learning in healthcare plays a pivotal role in fostering patient safety by making sure that healthcare professionals remain competent and adaptive to the best practices in the medical field. Outdated knowledge or skills in the medical field can directly jeopardize patient outcomes. Therefore, continuous professional development allows clinicians to update their professional competencies, reducing the risk of errors and adverse events.
This Collection invites research that examines how patient safety, which should be a professional expectation and ethical imperative at all stages of one’s career trajectory, can be enhanced through innovation in health professions education and training. Topics of interest include, but are not limited to:
• Tools and strategies for integrating patient safety into medical and nursing curricula
• Lifelong learning and continuing professional development (CPD) for patient safety and competence
• Simulation for teamwork, inclusion, and communication in diverse healthcare teams to enhance patient safety
• Interprofessional and collaborative safety culture
• Infection prevention and medication safety practices
• Learning from errors, near-misses, and real-time decision-making in clinical teams
• Strategies and policies for enhancing lifelong learning for patient safety
All manuscripts submitted to this journal, including those submitted to collections and special issues, are assessed in line with our editorial policies and the journal’s peer review process. Reviewers and editors are required to declare competing interests and can be excluded from the peer review process if a competing interest exists.
This Collection supports and amplifies research related to SDG 3: Good Health and Well-Being and SDG 4: Quality Education.
Publishing Model: Open Access
Deadline: Aug 18, 2026




Please sign in or register for FREE
If you are a registered user on Research Communities by Springer Nature, please sign in
🔹 "AMR is a growing global crisis, and tackling it starts with education! This study highlights the critical role of healthcare students in antibiotic stewardship. Great initiative!"
🔹 "Antibiotic misuse fuels resistance, yet awareness gaps persist among future healthcare providers. Studies like this are key to strengthening AMR education!"
🔹 "Educating healthcare students today means a stronger fight against AMR tomorrow. This research sheds light on an urgent issue—kudos to the team!"
Call to Action🔹 "Antimicrobial resistance is a major public health threat. How can we enhance AMR education among healthcare students? Let's discuss!"
🔹 "Addressing AMR requires collective action. What policies or interventions do you think could improve antibiotic stewardship in Nigeria?"