Unveiling the Hidden Burden of Pertussis in Adults
Published in Chemistry, Biomedical Research, and General & Internal Medicine

The Untold Story of Pertussis in Adults
Pertussis isn’t just a childhood disease. Adults with respiratory conditions like asthma or COPD are particularly vulnerable, yet pertussis often goes undiagnosed. My own experience as a pediatric resident exemplifies this: I endured months of a relentless cough that wasn’t identified as pertussis.
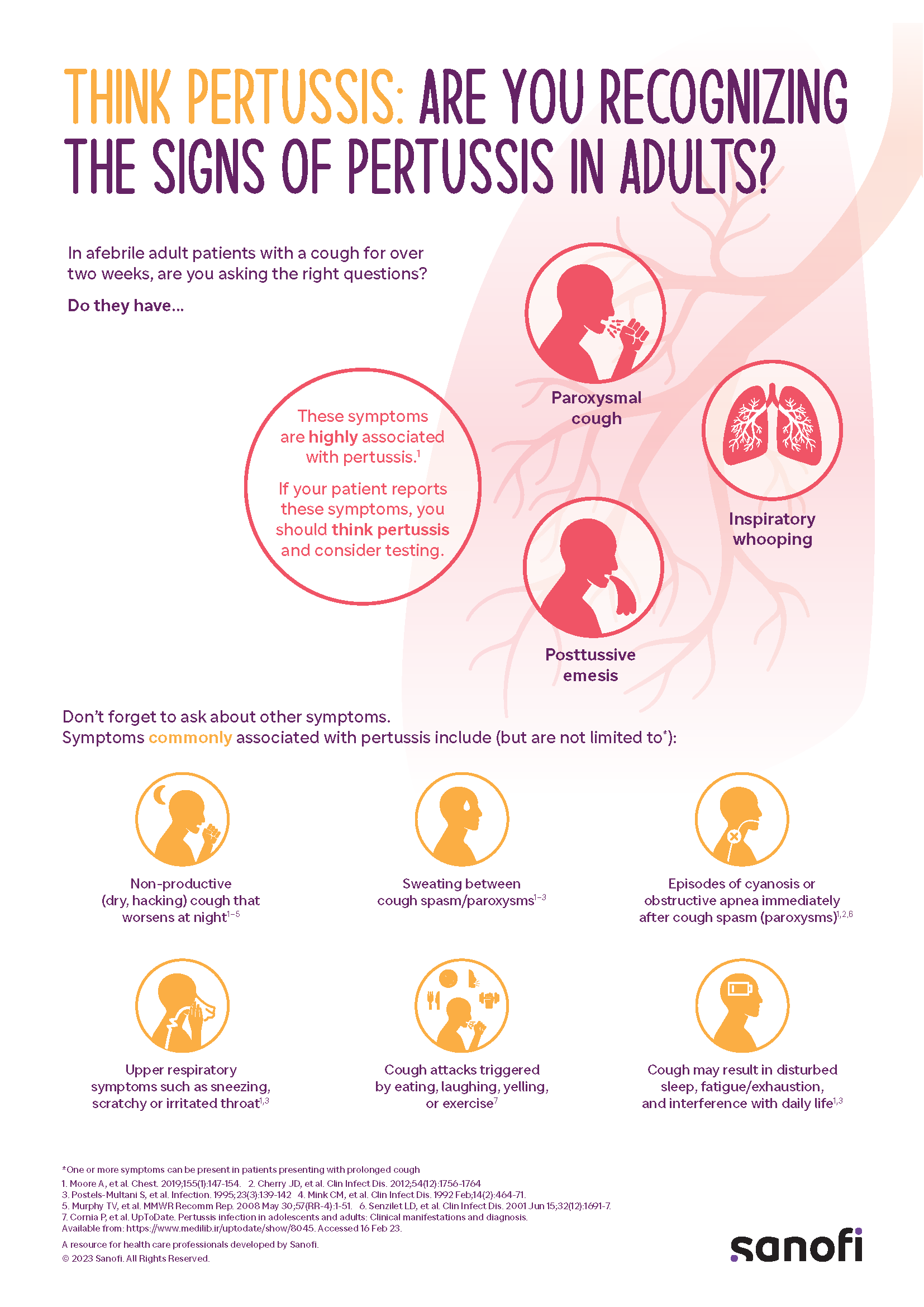
When I began working on pertussis at Sanofi, I quickly realized that most prevention efforts focus on children, especially young infants who are most vulnerable to severe complications. Yet, as a pediatric resident years ago, I experienced firsthand the devastating impact of pertussis in adults—though I didn’t know it at the time.
I vividly recall the ordeal: a relentless, hacking cough that lasted over three months, making sleep impossible and causing me to vomit after coughing fits. The doctors I consulted never considered pertussis as a diagnosis. Instead, I endured a battery of tests, including chest X-rays and arterial blood gases (a procedure I wouldn’t wish on anyone), without any answers. At one point, I was convinced I had contracted PPD negative tuberculosis.
It wasn’t until much later, as I learned more about pertussis in my work, that I realized I had been battling whooping cough all along. This revelation fueled my mission to ensure that pertussis is recognized as a significant health threat—not just for infants, but for people of all ages. Like many adults then and now, I had no idea that pertussis could affect me, and neither did the doctors treating me.
The Motivation Behind the Study
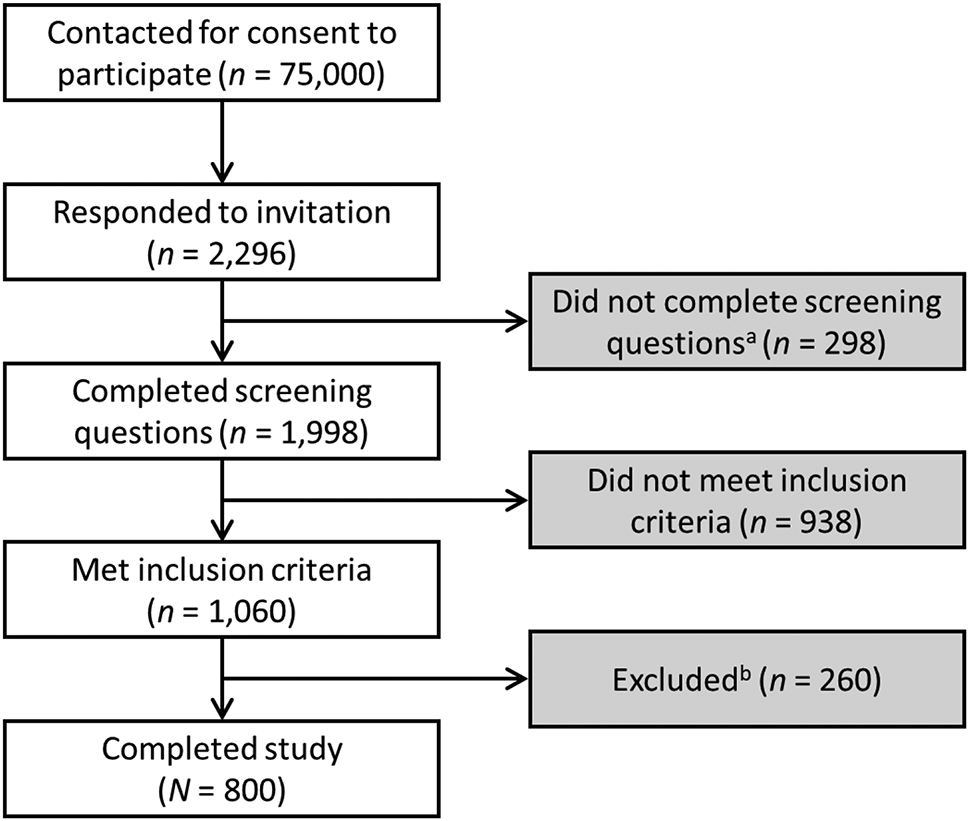
This gap in awareness is why our recently published study on pertussis vaccination in adults felt so personal. We surveyed over 800 physicians across the U.S., France, and Germany to understand their attitudes and practices around adult pertussis vaccination. What we found was disheartening: while physicians acknowledged the risks for certain high-risk groups, they ranked pertussis vaccination for adults as less important than tetanus.
When was the last time anyone saw a case of tetanus?
Overcoming Barriers to Vaccination
Physicians in our study highlighted a range of barriers to vaccination, including patients’ low perception of risk. Many adults simply don’t see themselves as vulnerable to pertussis, even though they’ve likely been vaccinated against tetanus—a disease far less common than pertussis.
Logistical hurdles also create challenges. In some countries, like France, patients must navigate a multi-step process to receive a vaccine, creating delays and missed opportunities. Even in places where access is easier, vaccine fatigue and competing health priorities can still impact uptake.
For healthcare providers, lack of educational tools and reminders can make it harder to integrate pertussis vaccination into routine care. Addressing these barriers is essential to improving vaccination rates and protecting adults from pertussis.
The Path Forward
This study underscores the need for greater awareness and education about pertussis in adults. We must empower physicians to recognize pertussis as a potential diagnosis in adult patients with persistent cough and to prioritize vaccination—not only to protect individuals but also to reduce community transmission.
For me, this isn’t just about data; it’s about ensuring that no one has to endure what I went through. Violently coughing for 100 days is more than a nuisance—it’s a public health issue that deserves our attention.
Follow the Topic
-
BMC Primary Care
Previously known as BMC Family Practice, this is an open access, peer-reviewed journal that considers articles on all aspects of primary health care research.
Your space to connect: The Primary immunodeficiency disorders Hub
A new Communities’ space to connect, collaborate, and explore research on Clinical Medicine, Immunology, and Diseases!
Continue reading announcementRelated Collections
With Collections, you can get published faster and increase your visibility.
Sleep health and primary care
Sleep health is a critical yet often overlooked aspect of overall well-being, particularly in the context of primary care. Sleep disorders, including insomnia and obstructive sleep apnea, can significantly impact patients' physical and mental health, leading to complications that may complicate primary care management. Sleep issues are becoming increasingly recognized for their chronicity, widespread prevalence, and influence on other chronic conditions. Therefore, understanding the relationship between sleep health and primary care practices is vital. This Collection aims to explore the intersection of sleep health and primary care, shedding light on innovative approaches to assessment and treatment.
Continued exploration in this area could pave the way for groundbreaking advancements in the management of sleep health care within primary care settings. As more research is conducted, we may see innovative approaches to screening and treating sleep disorders that can assist primary care providers in addressing these issues more effectively and efficiently. Future studies may also illuminate the impact of sleep health on chronic disease prevention and management, ultimately leading to a more holistic approach to patient care. By enhancing sleep health awareness among primary care providers, we can promote comprehensive care that acknowledges the crucial role of sleep.
We invite submissions on a range of topics that include, but are not limited to:
- Management of insomnia in primary care
- Management of obstructive sleep apnea in primary care
- The intersection between sleep disturbances and chronic disease
- Integrated behavioral health approaches to the management of sleep disorders
- Screening tools for sleep disorders in primary care
- Implementation of new models of care for sleep disorders
This Collection supports and amplifies research related to SDG 3: Good Health and Well-being.
All manuscripts submitted to this journal, including those submitted to collections and special issues, are assessed in line with our editorial policies and the journal’s peer review process. Reviewers and editors are required to declare competing interests and can be excluded from the peer review process if a competing interest exists.
Publishing Model: Open Access
Deadline: Jan 07, 2027
Managing substance use disorders
Substance use disorders are a multifaceted issue that poses significant challenges to primary care providers and the healthcare system at large. This Collection aims to explore various dimensions of substance use management, including the identification and treatment of drug, alcohol, and tobacco use disorders. Research that focuses on screening, diagnosis, and risk assessment in primary care settings is particularly valuable in understanding how to effectively manage these disorders and reduce their impact on individuals and communities.
Understanding and addressing substance use disorders is crucial for enhancing public health outcomes and ensuring the well-being of patients. Recent advances in screening tools and interventions have shown promise in identifying individuals at risk and providing them with appropriate support and treatment. By fostering collaboration between primary care providers, mental health professionals, and community organizations, we may witness a significant shift in how substance use is perceived and managed, ultimately improving health outcomes and quality of life for affected individuals.
We invite submissions on a range of topics that include but are not limited to:
- Innovative screening methods for substance use disorders
- Interventions for alcohol use disorders
- Management strategies for tobacco cessation
- Risk assessment approaches in primary care
All manuscripts submitted to this journal, including those submitted to collections and special issues, are assessed in line with our editorial policies and the journal’s peer review process. Reviewers and editors are required to declare competing interests and can be excluded from the peer review process if a competing interest exists.
Publishing Model: Open Access
Deadline: Sep 08, 2026


Please sign in or register for FREE
If you are a registered user on Research Communities by Springer Nature, please sign in