For many years, R-CHOP has remained the standard of care for patients with newly diagnosed diffuse large B-cell lymphoma. Numerous attempts to build upon its efficacy through the addition of novel agents have to date not improved overall survival, and in some cases have been hindered by excess toxicity.1-3
As with many cancers, there is evidence that the tumour-immune system impacts prognosis in DLBCL. Several mechanisms of “immune escape” have been described in DLBCL; increased expression of PD-1 and/or PD-L1 by lymphoma cells and the tumour microenvironment, mutations in and loss of heterozygosity of HLA-A, and mutations in other genes involved in antigen presentation.4, 5 Furthermore, an impaired anti-tumour immune response predicts for poor outcomes in DLBCL patients treated with chemotherapy.6, 7
Checkpoint inhibitors have revolutionised the treatment of many solid organ malignancies, but despite strong justification for their use single-agent checkpoint inhibitors have shown extremely limited efficacy in relapsed/refractory DLBCL.8 So why pursue checkpoint inhibition in treatment naïve patients? We felt that the timing of checkpoint inhibitor delivery was key, and thus designed a “window” study of sequential avelumab (PD-L1 inhibitor) and rituximab priming, R-CHOP and avelumab consolidation based on the following rationale:
- The immunosuppressive effect of prior therapy may have contributed to the lack of efficacy in heavily pre-treated relapsed/refractory DLBCL.
- Neoadjuvant checkpoint inhibition induces higher responses in chemotherapy-naive solid tumour patients, including subgroups not responsive to ICI in late-stage disease.9, 10
- Checkpoint inhibitors have seemingly re-sensitised relapsed DLBCL to subsequent chemotherapy in retrospective cohorts, a phenomenon described as “immune priming.”11
- Concurrent steroid administration may reduce the efficacy of checkpoint inhibition12
To our knowledge, our study was the first to evaluate a sequential, immune-priming strategy whereby a checkpoint inhibitor is delivered prior to and following R-CHOP chemotherapy in DLBCL. It thus also afforded the unique opportunity to observe the efficacy of checkpoint inhibition in checkpoint inhibitor naïve patients.
This sequential treatment protocol was safe, with no unexpected toxicity nor impact on R-CHOP delivery. Immune related adverse events (irAEs) were observed in 71% of patients, though these were generally mild with only one patient ceasing avelumab due to toxicity. The most common irAEs were rash (50%), thyroid dysfunction (29%), liver function derangement (18%) and arthralgias (18%). The safety profile was otherwise in keeping with expected R-CHOP toxicity.
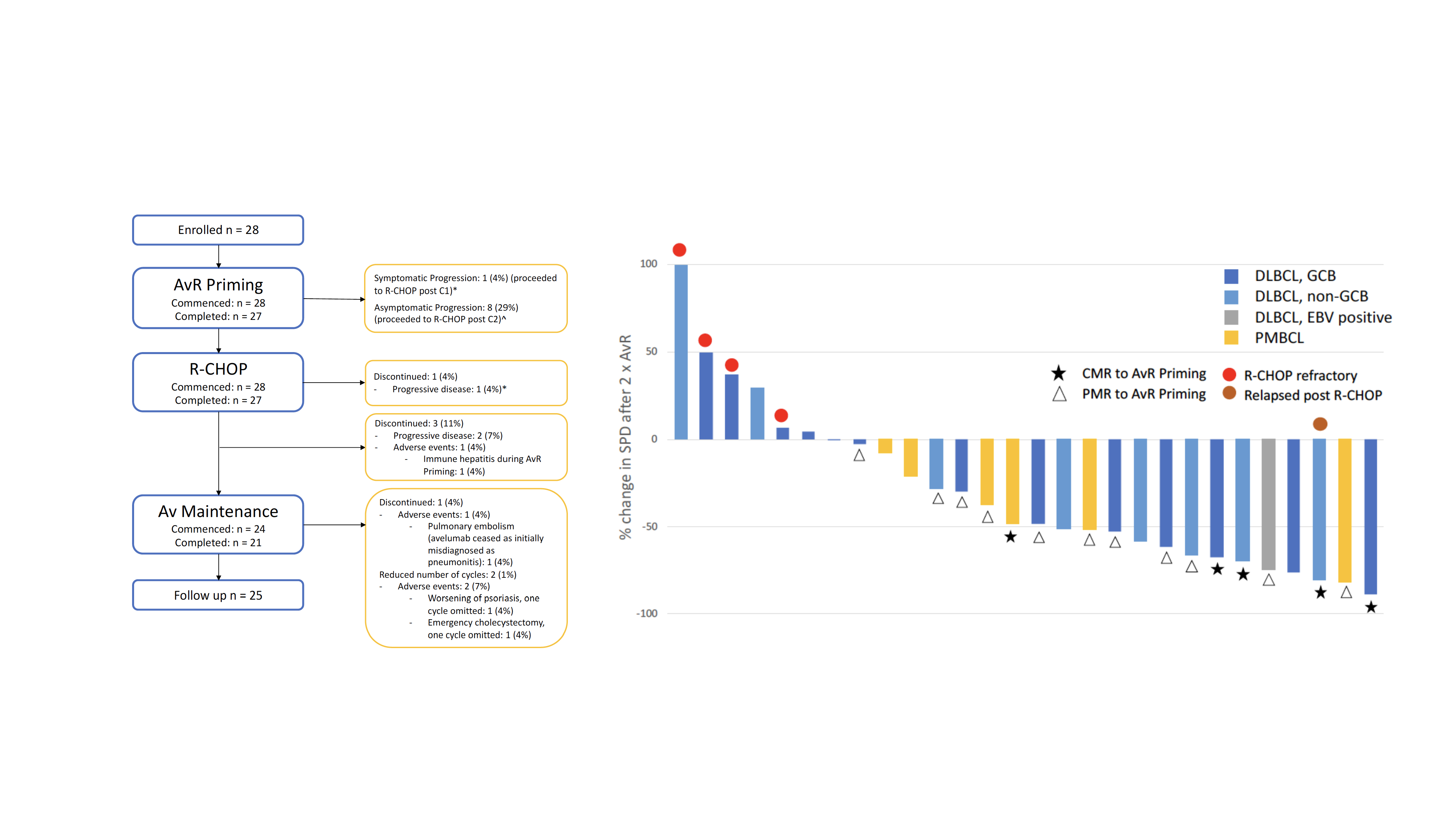
Acknowledging the limitations of a phase II study, promising efficacy signals were observed in all histological subgroups, but most notably primary mediastinal B-cell lymphoma (PMBCL) and EBV-positive lymphoma (subtypes known to be associated with increased PD-L1 expression through 9p24.1 aberrations and EBV-mediated activation of the JAK/STAT pathway respectively). The overall response rate to the avelumab and rituximab priming (AvRp) phase of 57% (complete response 18%) was higher than expected from rituximab alone, suggesting that checkpoint inhibitors may be more efficacious in the frontline setting compared with relapsed disease. The overall response rate following AvRp and R-CHOP of 89% (all CR) was also promising.
Of note however is the 32% of patients who progressed during the AvRp phase. Though some of these patients had potential “pseudoprogression” (discordant development of small new lesions with response in the majority of pre-existing tumour sites), 43% of those with unequivocal progression during AvRp were subsequently primary refractory to R-CHOP (OR=15; 95%CI:1.2-183.6; p=0.03). Patient selection for a sequential immune-based strategy is thus of critical importance. In our accompanying correlative studies we explored potential predictors of response to AvRp. Interestingly, expression of PD-1, PD-L1, PD-L2, CD4 and CD8 by gene expression profiling did not predict response, nor was 9p21.4 amplification a prerequisite for AvRp response. Further translational work to identify the patients most likely to benefit from checkpoint inhibition is ongoing.
Overall, our study demonstrates that there may still be a role for checkpoint inhibition in the treatment of newly diagnosed DLCBL. The Australasian Leukaemia and Lymphoma Group is now evaluating sequential immune-priming strategies in PMBCL (NHL35 ALLG-PACIFIC) and EBV-positive DLBCL (NHL36-TREBL-2) and we look forward to seeing the results of these studies.
- Younes A, Sehn LH, Johnson P, Zinzani PL, Hong X, Zhu J, et al. Randomized Phase III Trial of Ibrutinib and Rituximab Plus Cyclophosphamide, Doxorubicin, Vincristine, and Prednisone in Non-Germinal Center B-Cell Diffuse Large B-Cell Lymphoma. Journal of clinical oncology : official journal of the American Society of Clinical Oncology. 2019;37(15):1285-95.
- Tilly H, Morschhauser F, Sehn LH, Friedberg JW, Trněný M, Sharman JP, et al. Polatuzumab Vedotin in Previously Untreated Diffuse Large B-Cell Lymphoma. New England Journal of Medicine. 2021;386(4):351-63.
- Bartlett NL, Wilson WH, Jung SH, Hsi ED, Maurer MJ, Pederson LD, et al. Dose-Adjusted EPOCH-R Compared With R-CHOP as Frontline Therapy for Diffuse Large B-Cell Lymphoma: Clinical Outcomes of the Phase III Intergroup Trial Alliance/CALGB 50303. Journal of clinical oncology : official journal of the American Society of Clinical Oncology. 2019:Jco1801994.
- Keane C, Vari F, Hertzberg M, Cao KA, Green MR, Han E, et al. Ratios of T-cell immune effectors and checkpoint molecules as prognostic biomarkers in diffuse large B-cell lymphoma: a population-based study. Lancet Haematol. 2015;2(10):e445-55.
- Wise JF, Nakken S, Steen CB, Vodák D, Trøen G, Johannessen B, et al. Mutational dynamics and immune evasion in diffuse large B-cell lymphoma explored in a relapse-enriched patient series. Blood Advances. 2020;4(9):1859-66.
- Keane C, Tobin J, Gunawardana J, Francis S, Gifford G, Gabrielli S, et al. The tumour microenvironment is immuno-tolerogenic and a principal determinant of patient outcome in EBV-positive diffuse large B-cell lymphoma. European Journal of Haematology. 2019;103(3):200-7.
- Kiyasu J, Miyoshi H, Hirata A, Arakawa F, Ichikawa A, Niino D, et al. Expression of programmed cell death ligand 1 is associated with poor overall survival in patients with diffuse large B-cell lymphoma. Blood. 2015;126(19):2193-201.
- Ansell SM, Minnema MC, Johnson P, Timmerman JM, Armand P, Shipp MA, et al. Nivolumab for Relapsed/Refractory Diffuse Large B-Cell Lymphoma in Patients Ineligible for or Having Failed Autologous Transplantation: A Single-Arm, Phase II Study. Journal of clinical oncology : official journal of the American Society of Clinical Oncology. 2019;37(6):481-9.
- Forde PM, Chaft JE, Smith KN, Anagnostou V, Cottrell TR, Hellmann MD, et al. Neoadjuvant PD-1 Blockade in Resectable Lung Cancer. N Engl J Med. 2018;378(21):1976-86.
- Chalabi M, Fanchi LF, Dijkstra KK, Van den Berg JG, Aalbers AG, Sikorska K, et al. Neoadjuvant immunotherapy leads to pathological responses in MMR-proficient and MMR-deficient early-stage colon cancers. Nat Med. 2020;26(4):566-76.
- Carreau NA, Armand P, Merryman RW, Advani RH, Spinner MA, Herrera AF, et al. Checkpoint blockade treatment sensitises relapsed/refractory non-Hodgkin lymphoma to subsequent therapy. British Journal of Haematology. 2020;191(1):44-51.
- Bröckelmann PJ, Goergen H, Keller U, Meissner J, Ordemann R, Halbsguth TV, et al. Efficacy of Nivolumab and AVD in Early-Stage Unfavorable Classic Hodgkin Lymphoma: The Randomized Phase 2 German Hodgkin Study Group NIVAHL Trial. JAMA Oncology. 2020;6(6):872-80.
Follow the Topic
-
Leukemia
This journal publishes high quality, peer reviewed research that covers all aspects of the research and treatment of leukemia and allied diseases. Topics of interest include oncogenes, growth factors, stem cells, leukemia genomics, cell cycle, signal transduction and molecular targets for therapy.





Please sign in or register for FREE
If you are a registered user on Research Communities by Springer Nature, please sign in