Novel inhibitor of breast cancer stem cells overcomes chemotherapy resistant triple negative breast cancer
Published in Cancer

Approximately 10 - 15 % of diagnosed breast cancers are triple negative breast cancer (TNBC) (1, 2). Although TNBC is treated with standard chemotherapeutic drugs such as paclitaxel, the response is variable, and many patients still recur with metastatic disease that is often fatal (3, 4). Many TNBCs are clearly resistant to current therapeutic regimens. One driving factor behind chemoresistance and tumor aggressiveness of TNBC is breast cancer stem cells (BCSC). BCSCs have the ability to self-renew and represent a relatively quiescent subpopulation of tumor cells that can escape the effects of chemotherapy because of their slower rate of proliferation, expression of drug transporters that can expel chemotherapeutics and higher DNA repair potential (5, 6). BCSCs are identified as the CD44high/CD24low or ALDHhigh subpopulation, and existence of the cells with these hallmarks correlates with poor prognosis of TNBC patients (7). Therefore, targeted inhibition of BCSC could enhance the efficacy of chemotherapy and improve outcomes for patients diagnosed with aggressive TNBC.
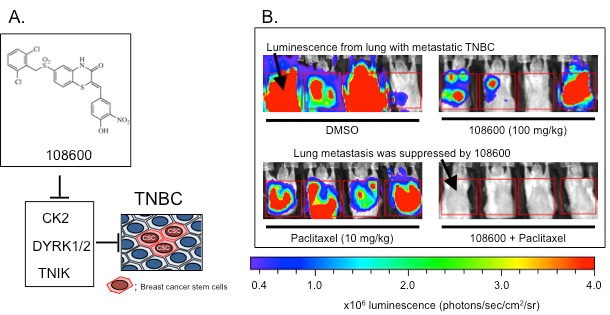
In this study, we functionally screened 4000 compounds for ability to inhibit and kill BCSC and discovered 108600. In vitro kinase profiling showed that the targets of 108600 are CK2 (Casein Kinase 2) DYRK1 (dual specificity tyrosine phosphorylation regulated kinase) and TNIK (TNF receptor associated factor 2 and NCK interacting kinase). CK2 interacts with AKT1 and Cyclin D1, and regulates cell cycle progression, apoptosis, energy metabolism, and DNA repair (8). DYRK1 is a regulator of quiescence, keeping cells in the G0/G1 phase (10) TNIK is an important regulator of WNT/β-catenin pathway; its interaction with TCF/LEF strongly promotes transcription of β-catenin target genes, such as c-MYC, Cyclin D1, and AXIN2 (11).
Although all three kinases have been reported to play a role in stem cell maintenance, there have been no previous simultaneous inhibitor. One of the key advantages of 108600 is its ability to suppress simultaneously and rather selectively, multiple pathways that promote survival of CSCs, avoiding the problem of redundant, compensatory signaling that compromised previous approaches.
In our studies, 108600 suppresses growth of patient-derived xenograft (PDX) tumor grafts derived from patient cancers that responded poorly to standard chemotherapy like paclitaxel. 108600 as a single agent or in synergistic combination with chemotherapy dramatically inhibited growth of these chemotherapy resistant tumors by decreasing the ALDHhigh subpopulation within these tumors. This was consistent with our hypothesis that inhibiting CSCs sensitizes cancers to chemotherapy. As we aim to move toward clinical translation to early phase trials, we tested the efficacy of 108600 against established TNBC metastases in mouse models, a scenario that simulates stage 4 TNBC disease in patients. Remarkably, combined 108600 and paclitaxel nearly completely eliminated metastases, supporting the promising potential of 108600 as an effective therapy for patients with advanced disease.
In addition to chemotherapy resistance, CSCs have also been associated with immune evasion. BCSCs could play a role in regulating the immune response to TNBC and could compromise the efficacy of immunotherapies that are increasingly used in the treatment of TNBC. Therefore, targeting BCSCs with 108600 could offer a novel strategy to enhance the efficacy of immunotherapeutics and we are actively pursuing these studies to evaluate its clinical potential.
- Dawson SJ, Provenzano E, Caldas C. Triple negative breast cancers: clinical and prognostic implications. Eur J Cancer. 2009;45 Suppl 1:27-40. doi:10.1016/S0959-8049(09)70013-9
- Lebert JM, Lester R, Powell E, Seal M, McCarthy J. Advances in the systemic treatment of triple-negative breast cancer. Curr Oncol. 2018;25(Suppl 1):S142-S150. doi:10.3747/co.25.3954
- Cortazar P, Zhang L, Untch M, et al. Pathological complete response and long-term clinical benefit in breast cancer: the CTNeoBC pooled analysis [published correction appears in Lancet. 2019 Mar 9;393(10175):986]. Lancet. 2014;384(9938):164-172. doi:10.1016/S0140-6736(13)62422-8
- Dent R, Trudeau M, Pritchard KI, et al. Triple-negative breast cancer: clinical features and patterns of recurrence. Clin Cancer Res. 2007;13(15 Pt 1):4429-4434. doi:10.1158/1078-0432.CCR-06-3045
- Yoshida GJ, Saya H. Therapeutic strategies targeting cancer stem cells. Cancer Sci. 2016;107(1):5-11. doi:10.1111/cas.12817
- Dean M, Fojo T, Bates S. Tumour stem cells and drug resistance. Nat Rev Cancer. 2005;5(4):275-284. doi:10.1038/nrc1590
- Visvader JE, Lindeman GJ. Cancer stem cells in solid tumours: accumulating evidence and unresolved questions. Nat Rev Cancer. 2008;8(10):755-768. doi:10.1038/nrc2499
- Rabalski AJ, Gyenis L, Litchfield DW. Molecular Pathways: Emergence of Protein Kinase CK2 (CSNK2) as a Potential Target to Inhibit Survival and DNA Damage Response and Repair Pathways in Cancer Cells. Clin Cancer Res. 2016;22(12):2840-2847. doi:10.1158/1078-0432.CCR-15-1314
- Liu R, Wang X, Chen GY, et al. The prognostic role of a gene signature from tumorigenic breast-cancer cells. N Engl J Med. 2007;356(3):217-226. doi:10.1056/NEJMoa063994
- Soppa U, Becker W. DYRK protein kinases. Curr Biol. 2015;25(12):R488-R489. doi:10.1016/j.cub.2015.02.067
- Mahmoudi T, Li VS, Ng SS, et al. The kinase TNIK is an essential activator of Wnt target genes. EMBO J. 2009;28(21):3329-3340. doi:10.1038/emboj.2009.285
Follow the Topic
-
Nature Communications
An open access, multidisciplinary journal dedicated to publishing high-quality research in all areas of the biological, health, physical, chemical and Earth sciences.
Related Collections
With Collections, you can get published faster and increase your visibility.
Women's Health
Publishing Model: Hybrid
Deadline: Ongoing
Biosensing
Publishing Model: Hybrid
Deadline: Jun 30, 2026






Please sign in or register for FREE
If you are a registered user on Research Communities by Springer Nature, please sign in