Physical exercise is recommended as part of standard care, with numerous studies establishing beneficial effects on physical function, treatment side effects and quality of life, particularly in patients with breast, colorectal and prostate cancer. However, as we delve deeper into this realm, a fundamental question emerges: can we extrapolate the efficacy of exercise interventions across various cancer types, or is there heterogeneity in effects highlighting a need for tailored approaches?
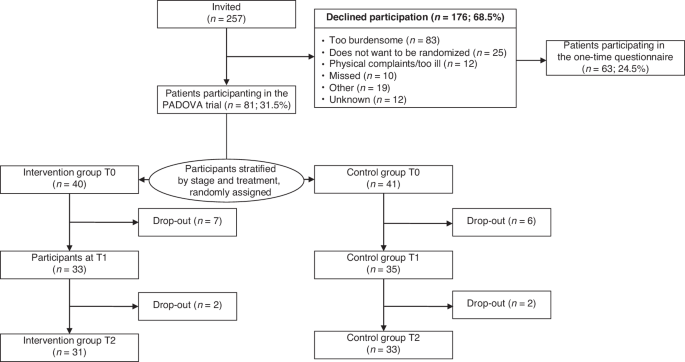
This query lies at the heart of our research journey, prompting us to challenge established norms and explore novel perspectives. While acknowledging the inherent differences among cancer types, such as detection stage and treatment modalities, we embarked on a randomized controlled trial to investigate the combined effect of a dietary and physical intervention during ovarian cancer treatment.
Our expectations were high, driven by the hypothesis that such interventions would yield tangible benefits, including improvements in physical fitness, fatigue management, and overall quality of life. And with baseline values that were worse than breast, colorectal and prostate cancer, even greater effects were able to be observed. However, our journey was fraught with challenges, including slow accrual rates and unforeseen outcomes.
Despite meticulous analysis and positive experiences by patients, we found no significant effect between the intervention and control groups. This revelation led us to introspect: were we measuring the right outcome? Did our quantitative metric capture the nuanced experiences reported in qualitative interviews? While quantitative analyses failed to demonstrate definitive benefits, qualitative insights unveiled a profound sense of empowerment amount the intervention group. Their narratives echoed feelings of resilience and adaptability in navigating the challenges of cancer treatment, contrasting with the sentiments of the control group.
This dissonance between quantitative data and qualitative narratives underscores the complexity of evaluating interventions in cancer care. While quantitative measures provide valuable insights, qualitative assessments offer a deeper understanding of patient experiences, including intangible aspects like empowerment. Empowerment can significantly impact a patients ability to adhere to treatment, and its value should not be underestimated. We need to better understand how empowerment can enhance treatment adherence and overall outcomes.
Moreover, the effects of exercise on cancer patients might not always follow traditional pathways, such as improved physical fitness. It’s crucial to explore whether alternative interventions would achieve the same results. Likely, they would not, as the unique value of exercise lies in its capacity to restore vigor and trust in one’s body. Physical exertion can rebuild lost confidence, providing sense of treat and reassurance in one’s physical capabilities. This renewed vigor can be crucial in helping patients maintain their treatment regimens and improve their overall well-being.
Navigating the publication process was equally illuminating, prompting us to strike a balance between nuance and clarity in conveying our findings. While the outcome may not align with conventional expectations, it serves as a valuable learning opportunity, shedding light on the multifaceted nature of cancer care.
As our findings enter the public domain, we remain steadfast in our commitment to exploring the role of physical exercise as a supportive element in cancer care. With gratitude, we acknowledge the acceptance of our paper by the esteemed British Journal of Cancer, signaling a step forward in our collective understanding of this complex landscape. Which brings us back to the question we started with: should we extrapolate the efficacy of physical exercise interventions across various cancer types, or is there a need for tailored approaches? We should be careful with extrapolating interventions across various cancer types.
Follow the Topic
-
British Journal of Cancer
This journal is devoted to publishing cutting edge discovery, translational and clinical cancer research across the broad spectrum of oncology.




Please sign in or register for FREE
If you are a registered user on Research Communities by Springer Nature, please sign in