Beyond the Diagnosis: How Financial Counselling Could Turn the Tide on Pakistan's Oral Cancer Crisis
Published in Cancer and Biomedical Research

As an Oral Surgeon and specialist in Oral Medicine with over two decades of clinical experience in Pakistan, I have seen the devastating, life-altering impact of oral cancer firsthand. It’s not just a medical statistic; it’s a patient losing their ability to speak, swallow, or smile, and a family facing immense emotional and financial distress. This reality is what motivates my research, particularly in addressing the primary culprit, Smokeless Tobacco (SLT).
The Unseen Burden of Addiction
In Pakistan, oral cancer is the leading cancer in males and the third most prevalent in females. Despite international efforts, SLT use remains rampant, particularly in rural communities where it is deeply ingrained in the cultural fabric.
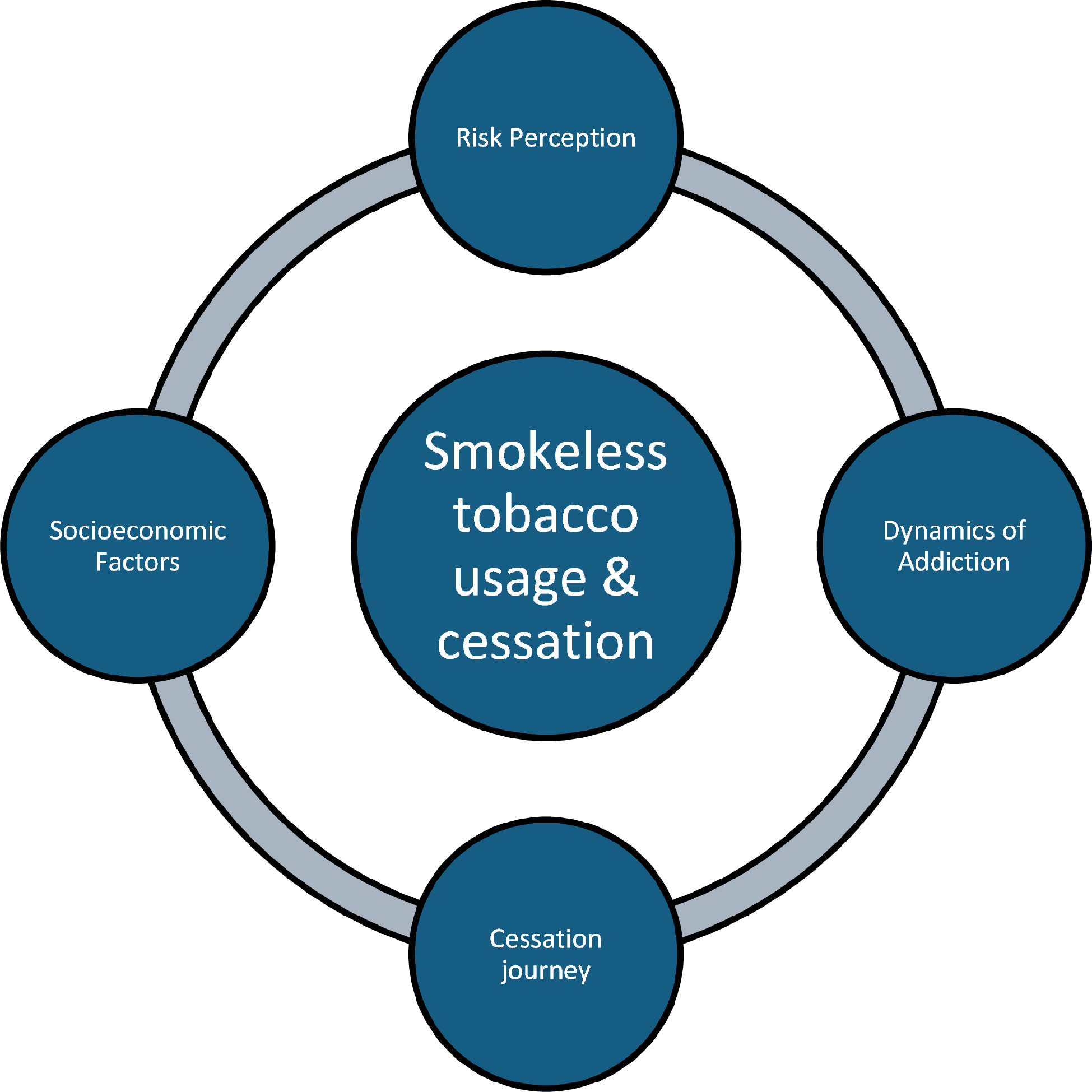
My co-authors and I recognized a crucial gap: while we treat the terminal outcome in the hospital, we rarely understand the deep socioeconomic and cultural roots that drive the habit in underserved areas. This led us to conduct a qualitative study in Gadap Town, a rural area near Karachi, to explore the lived experiences of SLT users.
The interviews revealed profound human stories that reflect what I suspect drives many of the cases I see clinically:
-
Emotional Dependency: Participants, especially women, described SLT as a coping mechanism for stress or a way to manage daily life challenges. They reported feelings of being trapped, with immediate relief overshadowing the long-term consequences. As one participant stated, "I need some to chew otherwise I don't feel like working".
-
The Awareness Gap: Even though participants were acutely aware that SLT "damages your teeth and cause cancer", this knowledge often coexisted with resignation or denial, resulting in a critical disconnect between health awareness and actual cessation behavior. They were simply too addicted to quit on their own.
The Role of Financial Counselling: A Potential Breakthrough Strategy
The most powerful finding in our research emerged from the intersection of addiction and poverty, the significant financial burden of the SLT habit. For low-income families in Gadap Town, where daily wages for unskilled workers may be as low as US$2.50 to US$5.00, the consistent purchase of products like Guthka created acute financial distress.
Participants frequently noted that daily expenditures on SLT detracted from essential family needs such as food, clothing, and education. This trade-off, a constant struggle between addiction and necessity, became a strong motivating factor for people to quit SLT use.
This insight suggests a potentially, highly effective avenue for intervention where traditional health warnings have failed, financial counselling.
Instead of solely focusing on the threat of cancer, interventions in rural settings should adapt behavior change strategies to emphasize the cost-saving benefits of cessation, directly linking quitting to improved quality of life and financial well-being for the entire household. This approach, such as tailoring the BISCA model (Behavioural Support Interventions for Smokeless Tobacco in South Asians), can turn economic strain from a household conflict into a powerful tool for behavioral change.
My team strongly advocates that training local healthcare workers in primary health care centers (PHCs) to routinely screen for SLT use and integrate this financial-focused counselling can make a critical difference in the success of cessation attempts in these marginalized communities.
Ultimately, overcoming Pakistan’s smokeless tobacco epidemic requires more than just clinical treatment; it requires targeted, culturally relevant, and financially sensitive strategies that address the full complexity of addiction as a socioeconomic problem.
Key Takeaways for Researchers and Policymakers:
-
Tailor Interventions: General health awareness campaigns are insufficient. Interventions must be culturally relevant and address emotional dependency and stress management.
-
Utilize Financial Leverage: Integrate financial counselling into cessation programs, emphasizing how quitting frees up household resources for essentials like nutrition and education.
-
Strengthen Regulation: Strict enforcement against the widespread availability of unregulated SLT is essential, as participants themselves believed a ban would be instrumental in helping them quit.
I welcome collaboration with researchers and policymakers interested in advancing these tailored, gender-sensitive interventions to finally reduce the devastating oral cancer burden in rural Pakistan.
Follow the Topic
-
BMC Oral Health
This is an open access, peer-reviewed journal that considers articles on all aspects of the prevention, diagnosis and management of disorders of the mouth, teeth and gums, as well as related molecular genetics, pathophysiology, and epidemiology.
Related Collections
With Collections, you can get published faster and increase your visibility.
Pregnancy and oral health
The relationship between pregnancy and oral health is an area of growing interest within dental and medical research. Pregnancy induces significant hormonal changes that can affect oral health, leading to conditions such as gingivitis and periodontitis. Additionally, pregnant individuals may face unique challenges in maintaining oral hygiene due to physical, emotional, and social factors. Understanding these interactions is crucial for developing targeted interventions that promote oral health during pregnancy, ultimately benefiting both the mother and the developing fetus.
Research has shown that poor oral health can lead to systemic complications, including adverse pregnancy outcomes such as preterm birth and low birth weight. Recent advances in this field include the development of tailored dental care guidelines and evidence-based interventions aimed at improving oral hygiene practices among pregnant individuals. Continued research can help bridge gaps in knowledge and practice, leading to better health outcomes for mothers and infants alike.
Ongoing exploration of the connections between oral health and pregnancy holds the promise of enhancing preventive strategies and interventions. By integrating dental care into prenatal healthcare, future studies may reveal innovative approaches to managing oral health concerns, ultimately contributing to healthier pregnancies and improved health outcomes.
We invite submissions on a range of topics that include, but are not limited to:
- Interventions for improving oral hygiene during pregnancy
- Impact of gingivitis on pregnancy outcomes
- Oral-systemic complications during pregnancy
- Importance of dental care in prenatal health
This Collection supports and amplifies research related to SDG 3: Good Health and Well-being.
All manuscripts submitted to this journal, including those submitted to collections and special issues, are assessed in line with our editorial policies and the journal’s peer review process. Reviewers and editors are required to declare competing interests and can be excluded from the peer review process if a competing interest exists.
Publishing Model: Open Access
Deadline: Jan 05, 2027
Patient satisfaction and prosthodontics
Patient satisfaction in the field of prosthodontics is a critical aspect that influences treatment outcomes and overall oral health. As dental professionals strive to enhance the quality of care, understanding the factors that contribute to patient satisfaction becomes essential. This Collection aims to explore the multifaceted relationship between prosthodontic treatments and patient experiences, examining how various factors—including communication, treatment options, and post-treatment care—impact satisfaction levels.
Recent advancements in prosthodontics, such as digital technologies, patient-centered care approaches, and improved materials, have shown promise in enhancing both functional and aesthetic results. By focusing on patient feedback and satisfaction metrics, practitioners can refine their techniques and improve the quality of care, ultimately leading to better health outcomes and increased patient loyalty. Continued research in this area may pave the way for the development of innovative assessment tools and methodologies that capture patient experiences more accurately. This could lead to the establishment of standardized benchmarks for patient satisfaction in prosthodontics, fostering an environment where patient-centered care becomes the norm rather than the exception.
We invite submissions on a range of topics that include but are not limited to:
- Assessing patient satisfaction in prosthodontic care
- Impact of treatment options on patient experiences
- Role of communication in patient satisfaction
- Advances in materials and their effect on satisfaction
- Patient-reported outcome measures (PROMs) and quality-of-life assessments in prosthodontics
- Psychological, social, and cultural determinants of patient satisfaction
- Satisfaction trends in geriatric, medically compromised, and special-needs patients
- Long-term satisfaction and maintenance-related factors in prosthodontic rehabilitation
All manuscripts submitted to this journal, including those submitted to collections and special issues, are assessed in line with our editorial policies and the journal’s peer review process. Reviewers and editors are required to declare competing interests and can be excluded from the peer review process if a competing interest exists.
Publishing Model: Open Access
Deadline: Oct 27, 2026




Please sign in or register for FREE
If you are a registered user on Research Communities by Springer Nature, please sign in